“Adrenal Fatigue”… “Adrenal Burnout”… “Adrenal Exhaustion.” That’s the story we’ve all been told about what causes chronic fatigue. It’s that chronic stress wears out our adrenal glands and causes them to be unable to produce enough cortisol, and then we get fatigue and all sorts of other symptoms. But is Adrenal Fatigue real?
Since the term “adrenal fatigue” was coined in 1998, the theory of adrenal fatigue has gained enormous popularity and is now believed by millions of people all over the world.
Yet, at the same time, “adrenal fatigue” is actually not accepted as a legitimate medical condition by conventional medicine. So how can it be that a theory which is so popular among natural health practitioners and millions of people in the general public not even be accepted as a real medical condition by conventional MDs?
Is adrenal fatigue real? Given how controversial this condition is, we need to take a closer look at the science to find out whether the research supports the idea that adrenal fatigue/cortisol abnormalities really are the major player in chronic fatigue.
This article is the most comprehensive analysis of the scientific research from the last 20 years that has examined the link between cortisol levels and chronic fatigue.
My hope is that this information will start to shift the paradigm among the natural health community, and to help individuals like yourself find the best, evidence-based path to fixing your fatigue.
Table of Contents
Download or listen on iTunes
Listen outside iTunes
What is Adrenal Fatigue? And What Are The Symptoms of Adrenal Fatigue?
For those that are unfamiliar with it, let’s do a quick overview of the theory of “adrenal fatigue.”
It is largely based on a researcher Hans Selye’s work from the 1930s-1950s, where he did testing on lab animals put under extreme stress. He found that they go through different phases of in their response when exposed to chronic stress, and then ultimately sort of shut down and are unable to maintain normal health – i.e. symptoms emerge. He proposed that these changes seemed to coincide with certain changes in hormones like adrenaline and cortisol along 3 specific phases, that ultimately ends in system-wide failure.
Adrenal fatigue proponents took Selye’s research and applied it to chronic stress in humans. Selye’s work was then used as support for the adrenal fatigue theory, and the idea that low cortisol (i.e. burned out adrenals) specifically is the fundamental cause of chronic fatigue and other symptoms that can emerge with chronic stress.
It generally is explained like this:
The adrenal glands produce stress hormones (like cortisol) to respond to periods of stress. Normally the system works just fine, but when the stress becomes chronic, the adrenal glands get worn out and “fatigued” so they can’t produce enough cortisol to keep up with the demands. Then you get fatigue and other symptoms.
The idea is that we go through a series of phases in response to chronic stress that looks like this:
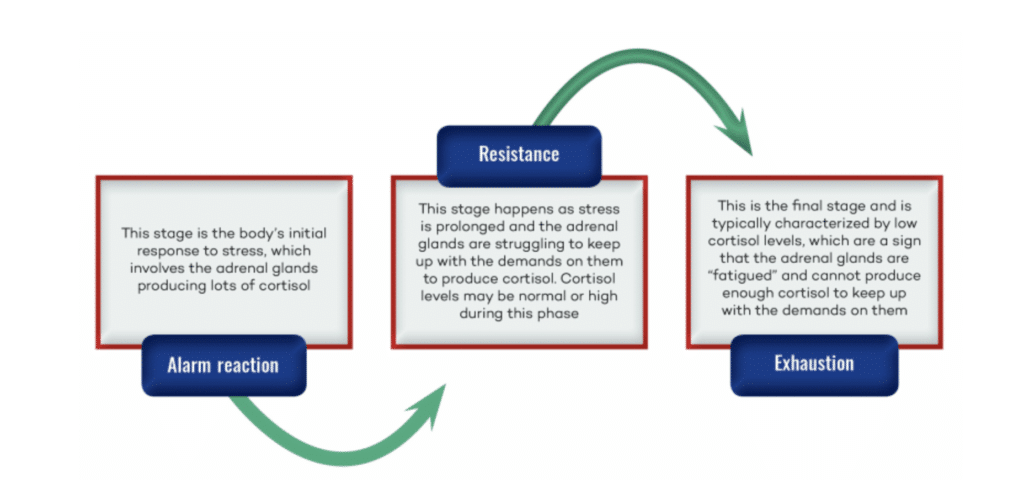
- Alarm reaction– This stage is the body’s initial response to stress, which involves the adrenal glands producing lots of cortisol.
- Resistance– This stage happens as stress is prolonged and the adrenal glands are struggling to keep up with the demands on them to produce cortisol. Cortisol levels may be normal or high during this phase.
- Exhaustion– This is final stage and is typically characterized by low cortisol levels, which are a sign that the adrenal glands are “fatigued” and can’t produce enough cortisol to keep up with the demands on them.
The third stage of “exhaustion” became known as “burnout” and then as “adrenal fatigue.”
The idea was that when your adrenal glands are “fatigued,” you get all sorts of symptoms like:
- Fatigue and lack of energy
- Depression
- Anxiety
- Brain fog
- Low blood sugar
- Low libido
- Waking up tired even after sleeping 7 or 8 hours
- Cravings for sugary and salty foods
- Trouble sleeping through the night (especially waking up between 2-4am)

That is the basic theory of adrenal fatigue. It seems like a logical concept, and perhaps that is why it has become such a popular idea.
While this theory of adrenal fatigue has many people who believe in it and preach it, there are numerous problems with it.
As you’re about to see, based on research that has been conducted over the last 25 years, the evidence simply does not support the idea that adrenal function and cortisol levels are key players in chronic fatigue.
The Two Schools of Thought on the Question “Is Adrenal Fatigue Real?” – The Conventional Doctors and the Holistic/Functional Health Practitioners
The concept of adrenal fatigue is commonly taught among naturalistic and holistic health practitioners, and is commonly believed by virtually all health seekers in the general public.
There are literally thousands of articles online and dozens of books written about “adrenal fatigue.” So of course, it must be a real thing, right?
Yet, if you are under that impression, it might interest you to know that adrenal fatigue is actually not even accepted as a legitimate medical condition by conventional medicine.
In fact, the Endocrine Society, representing 14,000 endocrinologists (doctors who specialize in hormonal health), has publicly stated:
“’Adrenal fatigue’ is not a real medical condition. There are no scientific facts to support the theory that long-term mental, emotional, or physical stress drains the adrenal glands and causes many common symptoms.” [1]
So there are basically two camps here:
- Adrenal fatigue proponents (most of the natural health community). These are the people writing articles and books about adrenal fatigue, and claiming to treat it. When asked “is adrenal fatigue real?”, they’ll likely chuckle at the thought that anyone could not believe it’s real, because they believe they see it in their clinics all the time.
- Conventional MDs. These people flat-out reject the notion that adrenal fatigue is legitimate medical condition. When asked “is adrenal fatigue real?”, they’ll most likely chuckle at the idea that anyone believes in it. They believe that the symptoms are not actually caused by poor adrenal function or cortisol issues, and that the science does not actually support the idea that the adrenals/cortisol is a significant cause of those symptoms.
Each group of people believes the other group is wrong and simply doesn’t understand what is really going on. Ask a conventional MD what they think of people who believe that adrenal fatigue is real and they’ll typically say that they’re quacks. Ask an adrenal fatigue proponent what they think of the conventional medical views on adrenal fatigue, and they’ll typically claim that it’s because the conventional medical world isn’t yet as scientifically advanced as they are, and hasn’t yet figured out that the adrenals and cortisol are behind the epidemic of chronic fatigue.
So what’s the truth here – is adrenal fatigue real?
Is “adrenal burnout” or “adrenal fatigue” or cortisol issues the real cause of your chronic fatigue?
That’s what this article will answer, by using the most comprehensive analysis of the science on this topic that has ever been done.
Get ready to be shocked, because the science in this area tells an amazing story of what is really going on in chronic fatigue.
The Story Behind Why I Developed The Ultimate Scientific Guide to Evaluate The Question “Is Adrenal Fatigue Real?”
Within the natural health community, we’ve all been told a narrative of how our adrenal glands and cortisol control our energy levels and are the cause of our fatigue. I myself was brought up with this concept in my education in holistic health. I read many books about adrenal fatigue, was taught about it from my mentors, and even taught the concept to my clients for many years.
So when I saw how so many conventional MDs were brushing off “adrenal fatigue” as nonsense, I had an idea to use the scientific evidence to prove that adrenal fatigue is real.
I originally started with a simple idea to compile the research in support of adrenal fatigue. I set out to write a book giving an overview of the last 20 years of research into the link between cortisol and fatigue.
My goal was simple: To prove scientifically that “adrenal fatigue” is real, is a legitimate medical condition, and that adrenal fatigue is indeed the primary cause of fatigue. If someone wanted to know “is adrenal fatigue real?”, I wanted to create the ultimate science-backed resource for them to know that it is real and backed by research.
So I dug into the research and read every study I could find that relates to the link between cortisol levels (i.e. adrenal function) and fatigue. It was a process that took over 6 months of digging through the full texts of hundreds of studies.
And while my original intention was to prove the adrenal fatigue theory, something peculiar happened along the way…
I discovered that the evidence is wildly contradictory, and simply put, doesn’t actually support the notion that cortisol issues (or adrenal function) is a primary cause of chronic fatigue.
I discovered that my assumptions about what I would find were simply… wrong.
Now, in this scenario, what most people typically do is they ignore the evidence that conflicts with their views and then they pay attention to and cherry-pick only the evidence that supports their preconceived notions.
But instead of doing that, I decided to do something much more difficult: I decided to admit that my preconceived notions were incorrect, and to rethink the causes of fatigue. Then, I decided to do a comprehensive review of every study ever done on this subject and then I would let the science itself tell me what to believe.
- If the science pointed to the notion that adrenal dysfunction/cortisol abnormalities are found in a large majority of people with chronic fatigue, I would have to conclude that cortisol issues are the primary cause (or at least major player) in fatigue.
- And if the science showed that adrenal dysfunction/cortisol abnormalities are not found in a majority of people with chronic fatigue, then we have to admit that the science doesn’t support the idea that adrenal fatigue is the primary reason for chronic fatigue.
In this article, I will share with you literally all of the studies that have examined the link between cortisol and chronic fatigue so you can decide for yourself what the science shows about the question “is adrenal fatigue real?”
It’s over 20 years of studies. And here’s the most important part: You can verify for yourself that I have not cherry-picked the data – what you’ll find here is literally every relevant study done on this topic during the last 20 years. Please feel free to search for relevant studies that haven’t been included here, if you doubt that I’ve included all the research.
This is a scientific review unlike anything that has ever been done before. I have looked extensively in all books on adrenal fatigue and all prominent articles written online, and I have not found a review of the scientific literature related to the concept of “adrenal fatigue” that is even 1/10th as comprehensive as what you’re about to read. This is the most comprehensive analysis of the science on the relationship between fatigue and cortisol that has ever been done.
No Science on “Adrenal Fatigue,” So We Must Look at Research on the 3 Accepted Fatigue Syndromes
There is one big problem with trying to review the science on the question “is adrenal fatigue real?”
There isn’t any actual research on adrenal fatigue.
Let me explain what I mean…
Think of a medical condition. Diabetes, stroke, Alzheimer’s, obesity, hypothyroidism, celiac disease, lung cancer, depression, schizophrenia, psoriasis, dementia, or even obscure ones like Sjogren’s syndrome.
Now go to Pubmed.com (it’s a database of virtually all studies in existence – like Google for scientific studies) and do a search for that condition. (Or feel free to try it with any condition you can think up!)
You’ll notice that between hundreds to thousands of studies will quickly appear for each and every one of those conditions.
Now, guess how many you’ll find if you look up “adrenal fatigue”?
Virtually none. (Feel free to check for yourself).
In fact, it’s actually worse than a mere case of there being no scientific research. Why? Because if you do that search, you’ll actually find negative scientific data. That is, you’ll find research examining adrenal fatigue that has concluded that adrenal fatigue is a myth that has no basis in science.
That systematic review of the scientific literature (all relevant studies on the topic) is even titled “Adrenal Fatigue Does Not Exist!”
I’m sure you can guess what the researchers found, but here’s their conclusion so you can read it for yourself:
“We found an almost systematic finding of conflicting results derived from most of the studies methods utilized, regardless of the validation and the quality of performed tests. Some limitations of the review include: (1) heterogeneity of the study design; (2) the descriptive nature of most studies; (3) the poor quality assessment of fatigue; (4) the use of an unsubstantiated methodology in terms of cortisol assessment (not endorsed by endocrinologists); (5) false premises leading to an incorrect sequence of research direction; and, (6) inappropriate/invalid conclusions regarding causality and association between different information.
… This systematic review proves that there is no substantiation that “adrenal fatigue” is an actual medical condition. Therefore, adrenal fatigue is still a myth.”[2]
In short, there is no body of scientific evidence on “adrenal fatigue.”
So here’s the big problem: How can one review the scientific research on a condition that has virtually no scientific research?
Here was the key breakthrough: Since we cannot examine research on “adrenal fatigue” per se, we have to search elsewhere for studies that have examined the link between cortisol levels and chronic fatigue.
Fortunately for us, it turns out that there are actually 3 related fatigue conditions that are legitimate, recognized medical conditions that have thousands of studies on them:
- Burnout Syndrome
- Vital exhaustion (or Exhaustion Disorder)
- Chronic Fatigue Syndrome/fibromyalgia
It’s worth noting that the symptoms of these conditions have tremendous overlap with symptoms that are said to be associated with “adrenal fatigue.”
1. Burnout Syndrome

Here’s a description of the symptoms of Burnout Syndrome:
- Chronic fatigue
- Insomnia
- Forgetfulness/impaired concentration and attention
- Physical symptoms
- Increased illness
- Loss of appetite
- Anxiety
- Depression
- Anger
Note that these symptoms overlap with the supposed symptoms of “adrenal fatigue.”
2. Vital Exhaustion (or Exhaustion Disorder)

“Vital Exhaustion (VE) has three defining characteristics:
- feelings of excessive fatigue and lack of energy,
- increasing irritability, and
- feelings of demoralization.”[3]
3. Chronic Fatigue Syndrome/Fibromyalgia
First, it’s important to recognize that Chronic Fatigue Syndrome and Fibromyalgia are recognized medical conditions by conventional medical doctors and there is a large body of scientific evidence on the subject. (That’s in stark contrast to the virtually nonexistent research on “adrenal fatigue.”)
Here are the symptoms of Chronic Fatigue Syndrome:

The symptoms of “adrenal fatigue” and “chronic fatigue syndrome” are nearly identical.
Now, consider some peculiar coincidences:
Now, the author at www.adrenaladvice.com did a very interesting experiment. He got data from WebMD where they did a survey of people with CFS to see how many of them had a particular symptom. (E.g. 65% of people with CFS reported difficulty sleeping). Then he decided to conduct the same study with people who were either diagnosed with “adrenal fatigue” or suspected they might have it. What he found was remarkable, as you’re about to see in the charts below. The amount of people with adrenal fatigue and CFS reporting symptoms was almost identical! [4]
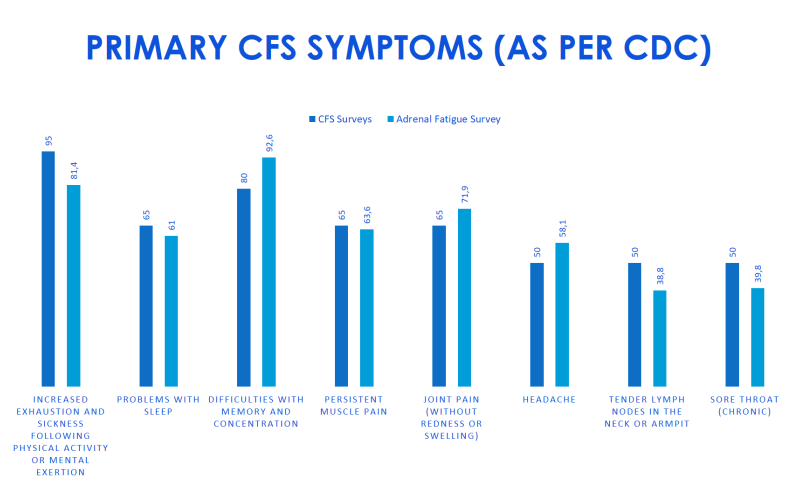
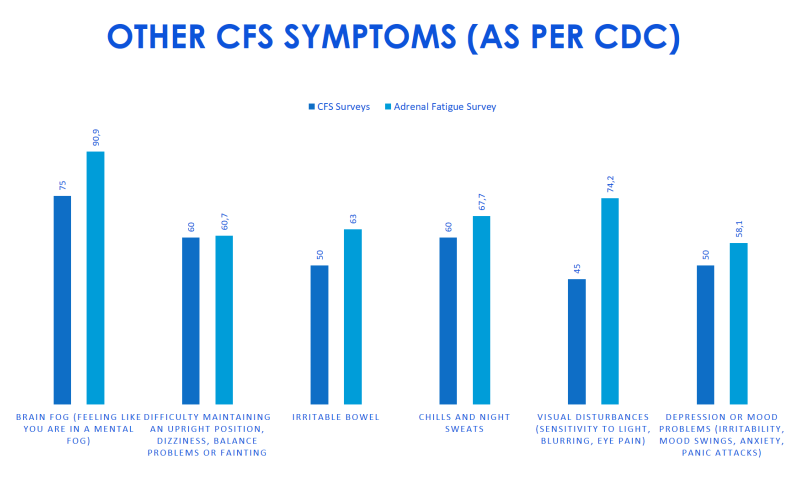
In other words, people diagnosed with adrenal fatigue (or those who self-diagnosed themselves with it) report the same symptoms as those with CFS! The percentages of each symptom are virtually the same!
Take a close look at the charts above. Do those really look like two different conditions? I think not.
Now, consider the fact there are no clear diagnostic tests specifically for either CFS or “adrenal fatigue.” Meaning, there isn’t any test in existence that one can get that would clearly get them diagnosed with CFS vs. Adrenal Fatigue. Diagnosis for both conditions tends to be done based on a process of elimination. In other words, the diagnosis is not by a diagnostic test – it’s made by ruling out other possible conditions. I.e. if you have these symptoms (like fatigue) and they do various tests and they don’t find any other disease, then maybe you have CFS or “Adrenal Fatigue.”
Because there is no clear diagnostic test, these people are all in no man’s land. That is, their condition is open to interpretation – and the conventional MDs are likely to give out a diagnosis of CFS whereas the alternative practitioners are likely to say it’s “adrenal fatigue.” (And people are likely to self-diagnose themselves with either adrenal fatigue or CFS, depending on what information they previously came across on the causes of fatigue). The point here is that there is no objective scientific test that can diagnose someone with either adrenal fatigue or CFS, let alone to distinguish between the two.
What I am suggesting here is that a huge proportion of people who have these symptoms are simply using different words for essentially the same thing.
- Alternative practitioners will say it’s “Adrenal Fatigue” and tell you the narrative of how chronic stress wears down your adrenals so they can’t produce enough cortisol.
- Conventional MDs will say it’s “Chronic Fatigue Syndrome” (or perhaps burnout syndrome or vital exhaustion).
So here’s the interesting part…
While there is virtually no research in existence on “adrenal fatigue,” there is actually a mountain of evidence from 20 years of research examining the relationship between these fatigue syndromes and adrenal function/cortisol levels.
So even though there is no research on “adrenal fatigue,” we can assess the validity of the theory of adrenal fatigue by looking at the dozens of studies that have examined the link between cortisol and chronic fatigue/vital exhaustion/burnout syndrome.
Based on the logical assumption that chronic stress might underlie these fatigue syndromes, researchers have been conducting well-controlled studies for over two decades to try to find a link between cortisol levels and fatigue syndromes. There are literally dozens of studies on this that have been conducted by researchers all over the world for over 20 years.
And, as you’re about to discover, the results of those studies are wildly contradictory, and the studies have failed to show that abnormal cortisol levels are the primary cause of these conditions.
Is Adrenal Fatigue Real? The Answer from 20 Years of Research Examining The Cortisol-Fatigue Link
As a whole, the research looking at these 3 fatigue syndromes and their relationship with adrenal function/cortisol levels is all over the place and is massively contradictory.
- Some studies are showing cortisol levels are higher in the morning…
- or lower in the morning…
- or higher all day long…
- or lower in the morning and higher at night…
- And the majority of studies show that there is no difference in cortisol between people who are burned out or chronically fatigued compared to those who are perfectly healthy.
To take this one step further, there are even studies which have examined the same people during burnout/chronic stress and after recovery from burnout/chronic stress that have shown:
- Decreased cortisol levels as symptoms improve
- Increased cortisol levels as symptoms improve
- No change in cortisol levels as symptoms improve
In short, with dozens of studies done on this topic by scientists all over the world for over 20 years, there is no consistent finding of any particular cortisol pattern that is associated with chronic fatigue.
Indeed, the data show that for the vast majority of people with chronic fatigue, there is no difference in adrenal function or cortisol levels at all when compared with normal healthy people.
I’m about to show you the summary of all of the 79 studies that have been done on this topic over the last two decades, but first, let’s just keep in mind the basic predictions of the “adrenal fatigue” theory. If adrenal fatigue is a real thing, it would mean that when we look at the research, we can expect to find a few things:
Adrenal Fatigue Predictions
If poor adrenal function/low cortisol were the primary cause (or even a major cause) of chronic fatigue/burnout…
- PREDICTION #1: We should find that all (or at least a large majority of) people with chronic fatigue/burnout have low cortisol levels (or at least some type of cortisol abnormality).
- PREDICTION #2: We should find low cortisol levels (or some type of cortisol abnormality) at the onset or early stages of chronic fatigue conditions.
- PREDICTION #3: We should see a reliable relationship where cortisol levels relate to symptoms. I.e. People with less severe symptoms have close to normal cortisol levels, and people with more severe symptoms have larger cortisol abnormalities.
- PREDICTION #4: We should see a reliable relationship where, as symptoms improve, so do cortisol levels.
- PREDICTION #5: We should find that raising cortisol levels should improve symptoms dramatically (as it does in true adrenal insufficiency/Addison’s disease).

As you’re about to discover, the actual evidence does not support any of these five basic predictions of the adrenal fatigue theory.
Now I’d like to actually show you all of the studies and what they found, so that you can come to your own answer to the question “is adrenal fatigue real?”
Let me emphasize again that this is essentially the entire body of scientific research examining the relationship of chronic stress and adrenal function. I.e. This is all the studies, so I’m not cherry picking the research to prove some theory—I’m showing you all the studies, including the minority of the studies which do show abnormal cortisol levels. When you look at all the studies – the entire body of evidence – it becomes readily apparent how contradictory all of the findings are. And specifically, it becomes apparent that cortisol abnormalities are not found at all in the majority of people with chronic fatigue or burnout.
Without further ado, here is the entire body of scientific research examining whether cortisol is linked with fatigue:

Now let’s look at the 20 systematic literature reviews on the link between chronic fatigue and cortisol levels.
The Systematic Literature Reviews on the Cortisol-Chronic Fatigue Link
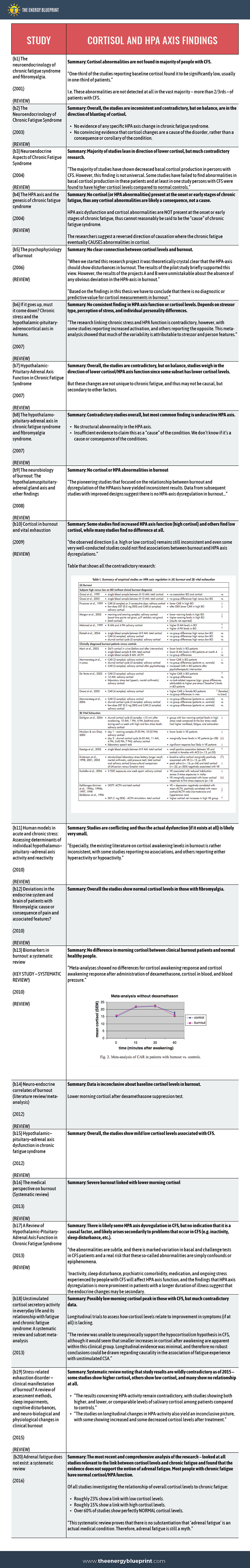
The Overall Body of Scientific Evidence – What do the 79 Studies Say About The Link Between Cortisol Levels and Fatigue?
59 individual studies and 20 literature reviews
- 15 of 59 studies give evidence for LOWER morning cortisol levels in people with chronic fatigue/fibromyalgia or burnout syndrome
- 11 of 59 studies give evidence for HIGHER morning cortisol levels in people with chronic fatigue/fibromyalgia or burnout syndrome
- 33 of 59 studies show no significant differences in cortisol levels in people with chronic fatigue/fibromyalgia or burnout syndrome (and/or that cortisol does not change as symptoms improve).
Evidence from intervention studies
- 10 studies overall
- 3 of the 10 studies showed a connection between cortisol increases and improvement in symptoms.
- 7 of the 10 studies showed no connection between fatigue and cortisol changes.
Evidence from 20 literature reviews
- The majority of reviews conclude that there are inconsistent and contradictory findings — i.e. some studies show high cortisol is linked with chronic fatigue/burnout, and others show low cortisol, and most do not find any cortisol abnormalities at all.
- The most common cortisol abnormality is in the direction of lower cortisol. But these changes are small and not found at all in a majority of studies.
- There is no specific cortisol pattern or change in HPA axis function that is unique to chronic fatigue/burnout.
- The majority of reviews conclude that people with chronic fatigue/burnout have no adrenal/HPA axis dysfunction and have normal cortisol levels.
A Deeper Look At Some of The Most Revealing Research on the Cortisol-Fatigue Link
Now let’s examine a few of the most impressive and revealing studies more in-depth.
Now let’s look at some systematic reviews (the highest level of scientific evidence) of the research on the link between HPA axis (hypothalamus-pituitary-adrenal axis, the whole network of brain regions that control adrenal cortisol output) function and chronic fatigue syndrome.
Speaking on the studies on burnout and cortisol levels, the researchers said:
“When taken together, among all the studies that investigated HPA-axis function and burnout, 3 support an INCREASE in HPA-axis functions in burnout, 5 support a DECREASE in HPA-axis functions, and 11 did not support a significant relationship.”[5]
They concluded:
“The pioneering studies that focused on the relationship between burnout and dysregulation of the HPA-axis have yielded inconsistent results. Data from subsequent studies with improved designs suggest there is no HPA-axis dysregulation in burnout…”[6]
HPA Axis dysfunction can be found in a small subset people with chronic fatigue syndrome. Even here though, the research is certainly not particularly compelling that HPA Dysfunction is the cause (or main mechanism) of why people get Chronic Fatigue Syndrome. In fact, the overall body of science makes the case that HPA Axis Dysfunction is likely a result – rather than a cause – of chronic fatigue.
A systematic literature review titled “The HPA axis and the genesis of chronic fatigue syndrome” reviewed the studies examining HPA Axis Dysfunction in CFS and concluded:
“Recent prospective studies of high-risk cohorts suggest that there are no HPA axis changes present during the early stages of the genesis of fatiguing illnesses.”[7]
Naturally, if HPA-Axis dysfunction were the cause of chronic fatigue, it should be present and detectable in the onset and early stages of the disease. In other words, if populations at high risk for getting chronic fatigue are analyzed, and the researchers can find no link between abnormal cortisol levels and a later risk of getting chronic fatigue syndrome, that is a good indication that cortisol levels/HPA function is not a significant causal factor. Moreover, if people who only recently developed chronic fatigue syndrome are analyzed and no cortisol/HPA abnormalities are found, that is also a good indication that cortisol/HPA function is not a significant player in the condition.
It’s not accurate to claim that something is the cause, when that thing isn’t even detectable at the onset or early stages of chronic fatigue.
The researchers also noted that HPA Axis Dysfunction is not present at all at the onset or during the early stages of CFS, and thus, the evidence doesn’t support the notion that HPA Axis Dysfunction is the cause. Moreover, they noted that just by correcting sleep patterns or through Cognitive Behavioral Therapy, the HPA Axis Dysfunction can be reversed – even as someone continues to experience the symptoms of CFS. Here’s what they wrote:
“In summary, evidence suggests that, although there is HPA axis disturbance present in subjects with operationally defined CFS, it is not present before the onset of CFS or during the early phases of illness, but develops once the illness has taken a more chronic course.”[7]
They concluded:
“A reversed direction of causation (i.e. that the illness leads to HPA axis change rather than the other way around) is supported by the findings that there is an apparent absence of HPA axis changes early in the genesis of chronic fatigue states, and that modifying cognitive behavioural components of the illness leads to a normalization of the HPA axis.”[8]
In short, there is no compelling case that adrenal dysfunction/HPA axis dyfunction/low cortisol levels are playing a significant causal role in chronic fatigue. It cannot be the primary cause of chronic fatigue, just by virtue of the simple facts that:
- It’s not present in the majority of people with chronic fatigue/burnout
- It’s not present during the onset or early stages of chronic fatigue/burnout
Naturally, if something is not even present at the onset or early stages of the actual condition it’s being claimed as a “cause” of, then one cannot reasonably claim it to be a “cause.” Moreover, if abnormal cortisol levels are claimed as the “cause” of a condition, and it is then discovered that a majority of people with that condition don’t actually have abnormal cortisol levels, then we know that abnormal cortisol levels are clearly not causing the condition.
Is Adrenal Fatigue Real? - Summary Of Research Findings:
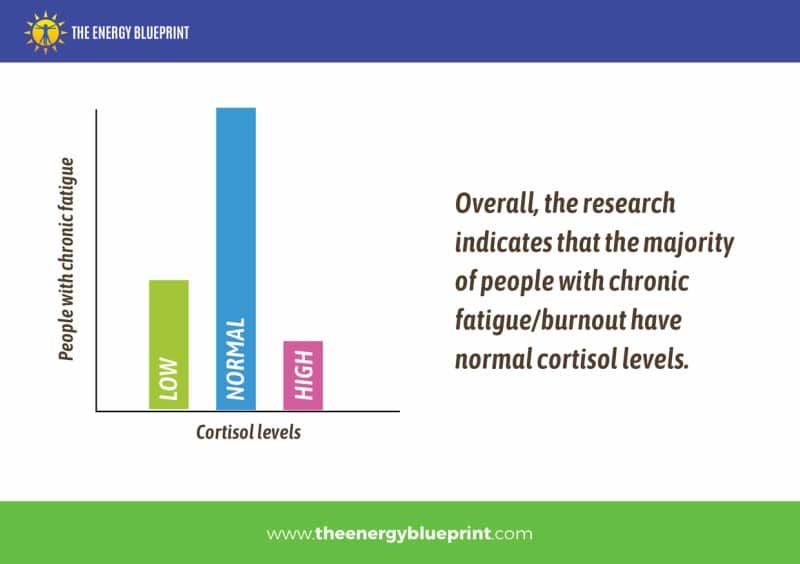
In summary, we can conclude with the following succinct summaries of the relevant literature:
- The majority of people with chronic fatigue/burnout appear to have perfectly normal cortisol levels. This is the most important point to grasp, because cortisol level abnormalities cannot possibly be “the cause” of a condition when most people with that condition don’t have cortisol abnormalities at all. Based on the research, we can estimate the percentages as follows:
- Roughly 20-30% of the overall population of those with chronic fatigue syndrome have lower morning cortisol (most studies indicate only very slight differences, still within the normal range)
- Roughly 10-15% of people with chronic fatigue syndrome have high morning cortisol (again, most studies indicate only very slight differences, still within the normal range)
- Roughly 65% or more of people with chronic fatigue syndrome have perfectly normal cortisol levels that are indistinguishable from normal healthy people.
- The overall body of evidence is contradictory. Studies find lower, higher, and perfectly normal cortisol levels in people with chronic fatigue/burnout. More than 20 years of research – over 60 studies, and 20 reviews of the scientific literature – have failed to generate any consensus about whether or not cortisol/HPA abnormalities even exist in chronic fatigue/burnout.
- A subset of people with chronic fatigue syndrome have low cortisol levels and blunted HPA axis activity. Overall, the evidence suggests this is the most common cortisol abnormality in chronic fatigue syndrome, among the minority of patients who have any cortisol abnormalities. (Remember, the majority of people with chronic fatigue have perfectly normal adrenal function and cortisol levels, and still another subset of people have the exact opposite cortisol abnormality).
- Cortisol/HPA axis dysfunction – even when they do occur in some people – are not present at the onset or early stages of the condition, and thus are likely not “causal.” (But it is certainly feasible that when cortisol abnormalities do occur, in a minority of people with chronic fatigue, they may act as a perpetuating factor in the condition that makes recovery more difficult).
- There is no specific change or pattern of HPA axis function or cortisol levels in either chronic fatigue syndrome or burnout syndrome. There is no specific pattern of cortisol/HPA dysfunction that is unique to chronic fatigue — the HPA axis abnormalities seen in some patients with chronic fatigue/burnout are also found in many other different conditions that have completely different types of symptoms. Thus, if cortisol levels or HPA axis dysfunction is claimed as a “cause” of chronic fatigue, it should be pointed out that it is extraordinarily unlikely that the same cortisol abnormalities could cause two (or 10) different types of conditions that have different sets of symptoms.
- There is a lack of longitudinal evidence that links cortisol changes to either worsening or improvement of chronic fatigue. There is little to no evidence that shows any kind of link between cortisol abnormalities causing chronic fatigue/burnout, as well as a lack of evidence showing that normalizing cortisol levels leads to improvement in chronic fatigue/burnout. In other words, more severe symptoms don’t typically relate to greater abnormalities in cortisol levels. And recovering from chronic fatigue/burnout is not typically paralleled by any changed in cortisol. In short, cortisol levels don’t appear to meaningfully relate to symptoms, and thus are unlikely to be the “cause” of those symptoms.
Does The Research Support The Predictions of Adrenal Fatigue or Not?
Please recall the 5 predictions of the theory of “adrenal fatigue” that we went over previously. As we can now see, none of the basic predictions of the “adrenal fatigue” theory are supported by the body of evidence.
- PREDICTION #1: We should find that all (or at least a large majority of) people with chronic fatigue/burnout have low cortisol levels. (NOT SUPPORTED BY THE EVIDENCE)
- PREDICTION #2: We should find low cortisol levels (or some type of cortisol abnormality) at the onset or early stages of chronic fatigue conditions. (NOT SUPPORTED BY THE EVIDENCE)
- PREDICTION #3: We should see a reliable relationship where cortisol levels relate to symptoms. I.e. People with less severe symptoms have close to normal cortisol levels, and people with more severe symptoms have larger cortisol abnormalities. (NOT SUPPORTED BY THE EVIDENCE)
- PREDICTION #4: We should see a reliable relationship where, as symptoms improve, so do cortisol levels. (NOT SUPPORTED BY THE EVIDENCE)
- PREDICTION #5: We should find that raising cortisol levels should improve symptoms dramatically (as it does in true adrenal insufficiency/Addison’s disease). (NOT SUPPORTED BY THE EVIDENCE)
In summary, the evidence does not support the theory that cortisol levels (or adrenal/HPA axis function) are a significant causal factor in chronic fatigue/burnout, and much evidence contradicts that conclusion.
The 4 Big Problems With The Theory Of “Adrenal Fatigue”
Beyond the simple fact that the research doesn’t support the notion that cortisol abnormalities have a clear link with chronic fatigue/burnout, there are also a number of other areas where the theory of “adrenal fatigue” is contradicted by the scientific evidence.
Specifically, there are four more big problems with the theory of adrenal fatigue.
Below are several pop-out boxes that go into detail on several other concepts showing that chronic fatigue is likely not being caused by any sort of adrenal dysfunction or cortisol abnormality.
PROBLEM 1 - Raising People's Cortisol Levels with Medication Doesn't Fix Their Symptoms (and Can Make Them Worse in the Long Run)
Here’s a simple way to test the theory of adrenal fatigue: If “fatigued” adrenals that aren’t producing enough cortisol is the fundamental cause of the symptoms, then increasing people’s cortisol levels should make them better.
For example, in true adrenal insufficiency/Addison’s disease (an accepted medical condition, in contrast to “adrenal fatigue) where people truly have low cortisol levels, we know that administering synthetic cortisol (e.g. hydrocortisone) actually does have amazing, life-transforming benefits. It is a life saver for people with low cortisol levels.
This is indeed a very simple way to test the theory. If low cortisol levels are truly the fundamental problem in chronic fatigue, then raising cortisol levels should fix the problem (just as it does in Addison’s disease). And many prominent proponents of “adrenal fatigue” actually do precisely that – they attempt to treat people with hydrocortisone or other forms of cortisone/cortisol to artificially raise cortisol levels.
This idea has actually been around for a long time. It was popularized by the book “Safe Uses of Cortisol” by Dr. William Jeffries.
Jeffries explained a concept the “adrenal insufficiency period,” which is essentially the same as “adrenal fatigue” – too little cortisol being produced by the adrenals. He talked about several different problems that were supposed to be associated with these low cortisol levels:

According to Jeffries, the problem here was too little cortisol, and thus, the solution he proposed was to administer synthetic cortisol (e.g. hydrocortisone) to increase a person’s cortisol levels.
Indeed, many alternative health practitioners still do use this approach, based on this thinking that lowered cortisol levels are causing the symptoms.
But the research shows that it doesn’t work, and that it often makes things much worse in the long-term.
It often does lead to some initial short-term success for a subset of patients. Likely because of two things:
- Cortisol is a powerful anti-inflammatory, so suppressing inflammation by pumping extra cortisol into the body can cause some initial benefits. (Think of how heroin or opium may have some initial benefits, but is not actually moving you towards health in the long run).
- The placebo effect will cause some subset of people to feel better with any medication (or even no medication at all – a sugar pill).
But what the research has shown is that when people with chronic fatigue (even the small segment who do have low morning cortisol levels) take external cortisol, it does not have significant benefit (and may even cause harm in the long run).
While initial studies seemed to potentially show some limited benefit[47] [48] (at least in the short-term), subsequent research which was more well-designed and longer term showed that taking more cortisol does not have benefit and may even cause worse outcomes in some people. Here are the results of the 3 studies conducted on this subject:
Study 1 – 70 patients were randomized to receive either hydrocortisone or placebo treatment for 3 months.[49] They found a significant improvement in 66.7% of patients taking hydrocortisone, and 54.3% of patients on placebo. Benefits were greater in the hydrocortisone group, but there was a remarkable amount of people reporting improvement on placebo, which is suspect. There was small improvement in a rating of “global health” but no significant change in ratings of fatigue for people taking hydrocortisone for 3 months.
Study 2 – 32 patients were put either on hydrocortisone or placebo for 28 days. 34% of patients on hydrocortisone reported a significant decrease in fatigue, compared with 13% reporting decreased fatigue while on the placebo.[50] While some patients reported reductions in fatigue, the researchers concluded “the majority of our sample gained little benefit from hydrocortisone…”
Study 3 – This was the most recent, the most well-designed, longest duration, and the most conclusive study.[51] It was a double-blind, placebo controlled, crossover-design 6-month study with 80 people with CFS. (Note: “Crossover” means that the same individuals spent 3 months on placebo and 3 months on the cortisone treatment). The study put people on 3 months of placebo treatment and 3 months of active treatment with hydrocortisone and fludrocortisone.
Remarkably, at the end of the 6 months, they found that raising cortisol levels did not improve symptoms – there was “no differences between treatment and placebo in patient-reported fatigue or well-being.”[52]
Importantly, they also noted that there weren’t even benefits to raising cortisol in the subgroup of patients with the lowest cortisol levels. The researchers explained:
“Finally, chronic fatigue syndrome is thought to be a heterogeneous disorder, and treatment with low-dose steroids may only be effective for a certain subset of patients (my note: i.e. those with lower cortisol levels). However, our treatment was not beneficial in patients with the lowest cortisol levels.” [53]
Another study confirmed this finding
“The patients with the lowest cortisol levels and adrenal reserve were not the most symptomatic, nor were they more likely to respond to hydrocortisone treatment.”[54
So even for that small subset of people with chronic fatigue who genuinely do have low cortisol levels, supplementing with external cortisol to raise cortisol levels back to normal still typically doesn’t give benefit.
Here are some conclusions from the studies which tested hydrocortisone treatment in people with chronic fatigue syndrome:
- “We found that low-dose hydrocortisone treatment has mild side effects and affords minimal therapeutic benefit for CFS, but significantly suppresses adrenal responsiveness.”[55] (Note: Your adrenal responsiveness is critical to coping with stressors, so it’s potentially very problematic to do things which prevent the body from adequately responding to stress).
- “Taken together, hydrocortisone replacement therapy cannot be recommended for clinical use because of the limited benefit, because of the loss of efficacy upon discontinuation and because of the adrenal suppression when using higher doses.”[56]
- “According to the stress crash theory, restoring HPA axis homeostasis…would revert the immune abnormalities observed in ME/CFS and thus improve the symptoms. However, the evidence supporting this stress crash or adrenal burnout hypothesis in ME/CFS is not strong. … treatment with hydrocortisone or fludrocortisone appears to have limited, mixed, or even adverse effects in ME/CFS.”[57]
Overall, the research does not support the idea that cortisol levels are the primary factor causing fatigue and other symptoms in people with chronic fatigue syndrome.
Correcting cortisol levels via medication does not improve fatigue for the vast majority of people. This is why it is not used as a treatment by virtually all evidence-based physicians.
Again, this suggests that:
- The body is intentionally lowering cortisol levels, and it’s not due to “adrenal burnout” preventing the adrenals from producing enough cortisol.
- Cortisol is not the primary cause of the symptoms in chronic fatigue.
Moreover, raising the body’s cortisol levels to a level higher than what the body is trying to maintain comes with a number of potential side effects:

Based on this research, what can we say about the question “is adrenal fatigue real?” Simply put:
- The reason why administering cortisol-raising treatments is not standard practice in medicine for treating chronic fatigue/burnout is because the research doesn’t support it.
- Correcting cortisol levels has little if any impact on the symptoms associated with chronic fatigue, even in the subset of chronically fatigued people with low cortisol levels. (And it can potentially cause problems).
- If raising cortisol levels back up to higher levels does not fix the chronic fatigue (or at the very least, provide significant benefit over a placebo), then low cortisol levels are clearly not the fundamental cause of the symptoms in chronic fatigue.
PROBLEM 2 - If a Potential Biomarker is Not Reliably Associated with a Specific Condition then it is Not a Valid Biomarker
As you’ve now seen, there is no particular cortisol abnormality that is reliably associated with fatigue. Indeed, the majority of studies show that the vast majority of people with fatigue have perfectly normal cortisol levels.
And yet, a large percentage of alternative health practitioners are attempting to diagnose a specific fatigue syndrome based on cortisol levels. (E.g. “Adrenal fatigue” and “adrenal burnout” and “adrenal exhaustion”).
This is pretty crazy if you think about it. There is no other condition in the world where people would insist on using a diagnostic marker that the research shows is so inaccurate and inconsistent.
When you’re looking for a diagnostic marker of a disease, you want to use some kind of marker that would show up on a test that would let you know if a person has a particular kind of illness. What you want to find is a reliable diagnostic marker that tells you whether or not someone has that condition.
This marker needs to be found in the large majority of people with that condition. And it needs to not be found in the majority of people without that condition.
Think about this scenario for a moment: Let’s say you wanted to have a test to see if people have insulin resistance/type II diabetes.
Now, let’s say you wanted to do this by looking at fasting blood sugar levels. (That is actually the primary thing physicians look at to assess insulin resistance). Of course, what you expect to find is that people with more insulin resistance have higher blood sugar levels.
Now let’s say you didn’t actually find that! Let’s you analyzed the blood sugar levels of thousands of people with type II diabetes and found that diabetics have:
- High blood sugar 25% of the time
- Low blood sugar 25% of the time
- Normal blood sugar 50% of the time
If that were the case, could you still use fasting blood sugar to diagnose insulin resistance?
Of course not!
This is basically the absolute worst diagnostic marker imaginable. They would never use a marker like that – they would throw it out immediately.
Why? Because they would recognize that it’s obviously not a valid marker to know whether or not someone has that condition!
Yet, that’s exactly what is going on with “adrenal fatigue.” Many practitioners are trying to use a diagnostic marker (cortisol) which simply does not have a reliable relationship to fatigue.
There is no other condition in the world where people would claim to use a diagnostic marker for a condition that is claimed to be sometimes high in the condition, sometimes low, and sometimes normal. In such a scenario, it would immediately be recognized that the biomarker is an invalid way of diagnosing the condition.
PROBLEM 3 - In Chronically Fatigued Persons with Low Cortisol, the Hormonal Profile Indicates that the Body is Intentionally Lowering Cortisol Levels, Not that the Adrenal Glands are "Fatigued" and Can't Produce Enough Cortisol
Based on the research into the hormonal profiles of people with chronic fatigue, even in those who do actually have low cortisol levels, the indications are that the body isn’t producing less cortisol because it can’t produce enough (i.e. because the adrenals are “fatigued” as a result of chronic stress), but because the body is instentionally lowering cortisol levels.
This is a critical point that often goes unnoticed.
To understand this, it requires a bit of understanding of how the HPA axis works.
In short…
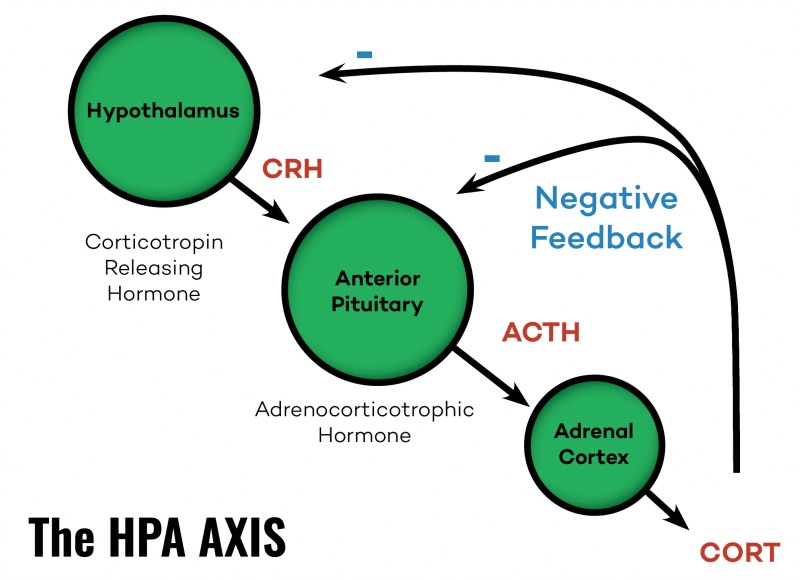
- Corticotropin Releasing Hormone (CRH) is produced by the hypothalamus
- Adrenocorticotrophic Hormone (ACTH) is produced by the pituitary
- Cortisol is released by the adrenal glands
The key point here is that the adrenals (i.e. cortisol levels) are being regulated by the hypothalamus and pituitary.
Once we understand this, it tells us something critically important about whether the low cortisol levels are caused by adrenals that are failing to make enough cortisol or if it’s because the brain is intentionally telling the adrenals to produce less cortisol.
See, in Addison’s Disease (true adrenal insufficiency), it is truly a case of the adrenals not being able to produce enough cortisol.
How do we know this?
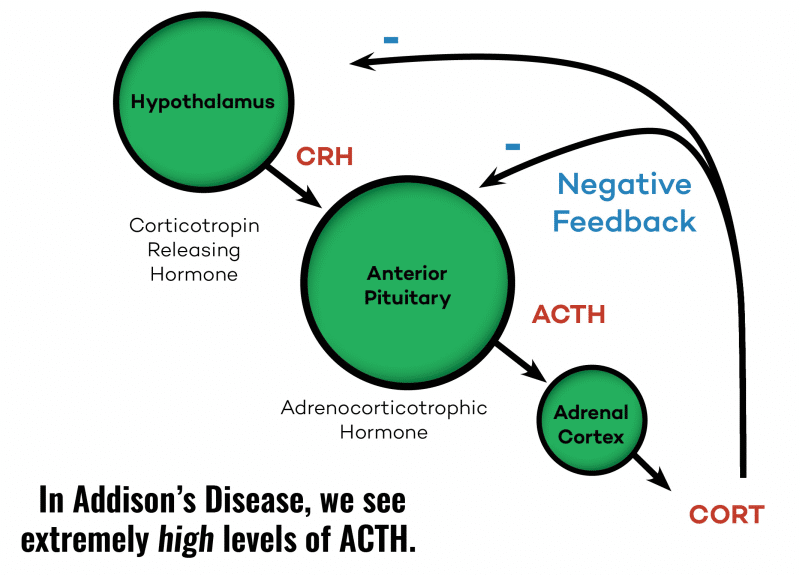
Because in Addison’s Disease, we see extremely high levels of ACTH.
What does that mean?
It means that the brain is screaming as loud as it can at the adrenals trying to get them to pump out more cortisol. Normally, more ACTH would lead to higher cortisol levels. But in Addison’s, the adrenals cannot respond to the ACTH signal and cannot produce enough cortisol.
So we see a clear pattern of:
- High ACTH (i.e. the brain trying to get the adrenals to produce more cortisol)
- Low cortisol (i.e. the adrenals can’t produce enough cortisol)
In burnout and chronic fatigue syndrome, we do not see this pattern at all.
- As explained in the research above, most studies indicate perfectly normal cortisol.
- Even in the small subset of people with lowered cortisol levels, we see normal or close to normal ACTH.
In other words, we clearly do not see a pattern of the brain calling for more cortisol to be produced and the adrenals not being able to produce it.
In addition, we also know from research on people with chronic fatigue that even low doses of hydrocortisone (which raises cortisol levels) suppress the body’s own production of cortisol.[10] What that clearly indicates is that the body wants cortisol levels exactly where they are, and trying to raise cortisol will cause the body to fight back and lower its production of cortisol even more.
If the adrenals were “fatigued” and unable to produce enough cortisol, we would expect to see that:
- ACTH levels should be high. (They’re not high).
- Raising cortisol (via hydrocortisone) to normal levels should produce dramatic benefits, and should not suppress the body’s own production of cortisol. (But it doesn’t have either of these effects).
In other words, the body is clearly making precisely the amount of cortisol that it wants to have – no more, and no less.
So what this means is that in the subset of people with lowered cortisol levels, it appears that the body is intentionally lowering cortisol levels.
This may be for several possible reasons:
- The body may intentionally lower cortisol to allow the body’s immune and inflammatory system to function in the face of threats: If there are chronic infections and/or toxins being put into the body, cortisol can suppress the immune response too much. Thus in situations where there is a chronic infection present or chronic toxin exposure, the body may intentionally lower cortisol to allow the body’s immune and inflammatory response to function properly.[11] In a recent 2016 study, researchers sought to determine whether the underlying cause in chronic fatigue syndrome is cortisol/HPA dysfunction, or inflammation and oxidative stress. And they showed that the inflammation and oxidative stress causes the HPA axis dysfunction, rather than the other way around. Research has indeed shown that the HPA axis is downregulated in response to chronic inflammation.
“The downregulation of the HPA axis in the face of a chronic inflammatory environment is well documented. The HPA axis becomes hyporesponsive following prolonged exposure to the cytokines, and this adaptation occurs relatively quickly.”
The researchers concluded:
“The stress crash theory that HPA axis hypofunction drives the activation of immune-inflammatory pathways in ME/CFS cannot be validated. This theory is contradicted by a number of findings, including (a) HPA axis hypofunction is only present in a subgroup of patients, (b) there are no changes in HPA axis during the early stages of ME/CFS, and (c) the immunosuppressive effects of GCs are enhanced in ME/CFS. On the contrary, we propose that HPA axis hypofunction in ME/CFS may be explained by a number of mechanisms, namely (a) chronic inflammation, through increased levels of TNFα; (b) a Treg response with elevated levels of IL-10 and TGF-β that is evident in some ME/CFS patients; (c) increased activity of (oxidative and nitrosative (O&NS) pathways, especially increased nitric oxide (NO) production; and (d) the effects of infection-related mechanisms that can downregulate HPA axis activity, such as LPS tolerance and viral infections…
HPA axis hypoactivity in ME/CFS is most likely a consequence and not a cause of a wide variety of activated immune-inflammatory and O&NS pathways in that illness.”[12]
If one is going to point the finger at some underlying cause, chronic inflammation and oxidative stress are likely better places to look than adrenal/cortisol changes. And to go one step further, the factors causing the inflammatory/oxidative changes.
- The body may intentionally lower cortisol as a simple consequence of poor sleep and certain lifestyle factors: Research indicates that lowered morning cortisol is not causal in fatigue syndromes, but likely arises as a consequence of a person’s behaviors, physical traits, or the very symptoms of the disease – e.g. disrupted sleep, medications, sedentary lifestyle, or simply being overweight.[13],[14] (We will discuss this in more detail in the next section).
- The body may intentionally lower cortisol as a way to facilitate the body’s healing response: Some hormone specialists have suggested that lowering cortisol levels is part of the body’s healing response, and that downregulation of the entire HPA axis is part of what happens when the body simply slows everything down to allow healing to occur.[15] (It is hard to objectively validate this with research, but it meshes well with the science and the experience of many clinicians who treat fatigue).
- The body may intentionally lower cortisol as part of the body’s downregulation of all many physiological systems in chronic fatigue: Research indicates that chronic fatigue is associated with a systemic, whole-body lowering of metabolic rate and energy production.[16]Essentially, this research suggests that virtually all of the functions of the entire body slow down in chronic fatigue. So in this case, lowered cortisol levels are potentially just one of hundreds of lowered chemicals in the body that can occur in chronic fatigue. (Interestingly enough, the study which found this body-wide shutdown of the metabolism actually found normal cortisol levels in people with chronic fatigue, despite hundreds of other metabolic markers being downregulated. [17] So even here, we get more evidence that cortisol levels are not a major player in chronic fatigue.)
In short, the actual hormonal profile of fatigued persons who have low cortisol does not support the notion that their adrenals are “fatigued” and cannot produce enough cortisol.
Rather, it indicates that the body wants cortisol levels exactly where they are, and is not attempting to make any more cortisol.
PROBLEM 4 - The Same Exact Cortisol Pattern That is Claimed By Some to Be Associated with Chronic Fatigue/Burnout is Also Found in People who Are Simply Overweight "20Night Owls" on Antidepressants or Simply Sleep Deprived
We have now seen that while most people with chronic fatigue/burnout have perfectly normal cortisol levels, there is a small subset of fatigued people with lowered morning cortisol levels.
The best estimate, from one review of the research is that 1/3rd of studies find lowered morning cortisol levels in roughly 1/3rd of people with CFS. (Note: If you do the math on that, it works out to be roughly 1/9th of overall people with chronic fatigue. But let’s be generous and estimate that it’s somewhere between 15-30% of people with chronic fatigue that have lower morning cortisol levels.)
To be more specific, the studies which have shown this cortisol abnormality have generally shown that it is specifically the morning cortisol awakening response that differs. (Even in these studies, most of them indicate that cortisol levels at all other times of day are perfectly normal, and that total cortisol output over 24 hours is also normal). And to get even more specific, the claim is that these people have a smaller peak in the rise in morning cortisol levels.
So one could perhaps reasonably believe from this that the lower morning peak in cortisol is a sign of “fatigued adrenal glands” that can’t produce enough cortisol, and that this is the real issue causing the symptoms of chronic fatigue/burnout (as some proponents of adrenal fatigue have).
Except there are several big problems with assuming that this cortisol pattern is a causal factor in chronic fatigue…
- This same exact cortisol pattern is also found in numerous other groups of people without chronic fatigue/burnout.
- The same exact cortisol pattern can be caused within days of engaging in simple behaviors (i.e. it is not caused by “adrenal exhaustion”).
- And the same exact cortisol pattern can be caused by some of the very symptoms of chronic fatigue syndrome.
As one research review put it:
“There is also no convincing evidence that any HPA axis changes are specific to CFS or a primary cause of the disorder rather than being related to the many possible consequences or corollaries of the illness.”[18]
There are numerous factors that will, by themselves – i.e. without chronic fatigue – cause the exact same cortisol pattern of a low morning peak in cortisol:
1. Excess body fat (i.e. being overweight)
Research has shown that the more overweight someone is, the lower their morning peak in cortisol will be.[19]
Here is the graph from the key study on this topic:
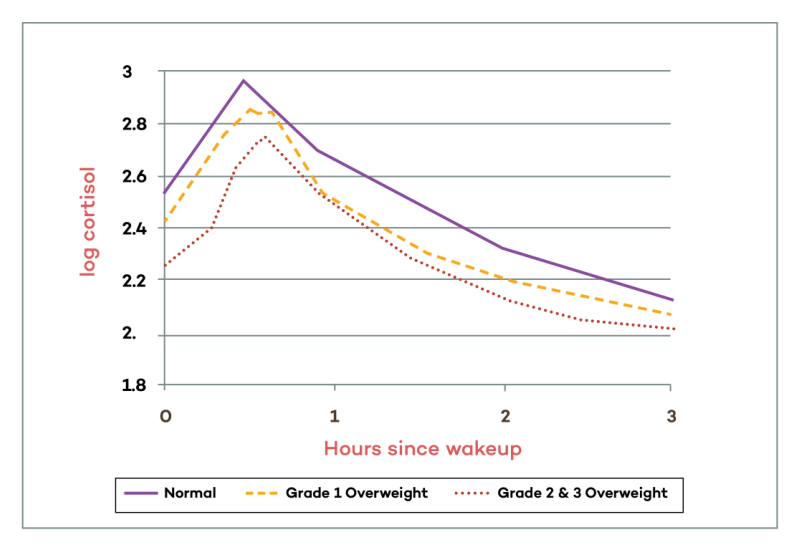
You can see clearly that being slightly overweight causes a slight lowering of morning cortisol, and being significantly overweight causes an even lower peak in morning cortisol levels.
Is the low morning cortisol a sign of chronic stress exhausting the adrenals, or simply being overweight?
2. Night owl chronotype (i.e. staying up later)
You can see here from this graph how one key study showed that night owls (evening types) have the same exact low morning peak in cortisol.[20]
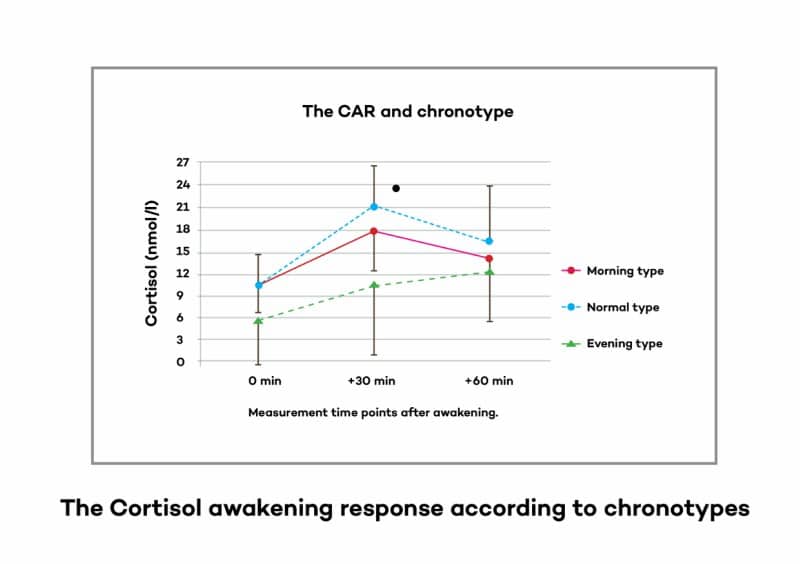
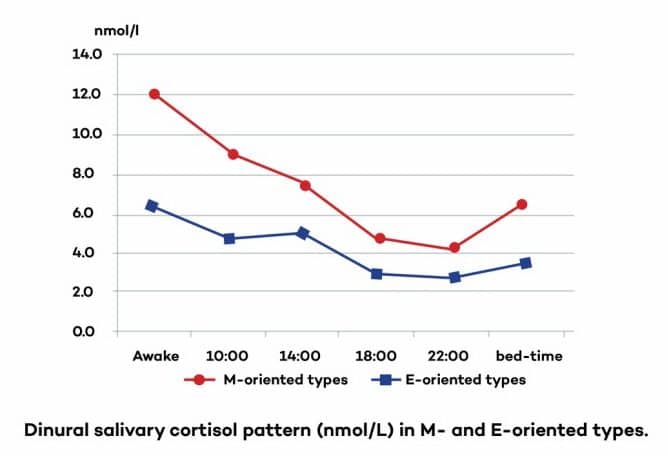
So again, the simple trait of being a night owl is, by itself, enough to explain why a subset of people with chronic fatigue/burnout have this cortisol pattern.
Moreover, research has also shown that being a night owl is associated with many other illnesses, including burnout.[28][29][30] Research has also shown that people with CFS tend to have disrupted circadian rhythm, which will lead to this cortisol pattern.[31]
So it is likely that a sizable portion of people with burnout/chronic fatigue are night owls, and have this cortisol pattern simply because they are night owls.
3. Night eating
Research has also shown that the simple habit of late night eating will cause a lower peak in morning cortisol levels.[32]
4. Antidepressant use
Several different types of prescription and over-the-counter drugs can affect morning cortisol levels. One example is some types of antidepressants.
Here is a graph from one study that showed a lower peak in morning cortisol in people on antidepressants.[33]
This graph illustrates the morning cortisol awakening response in a group of people with stress-related exhaustion, that only differed based on whether they were on antidepressants or not.
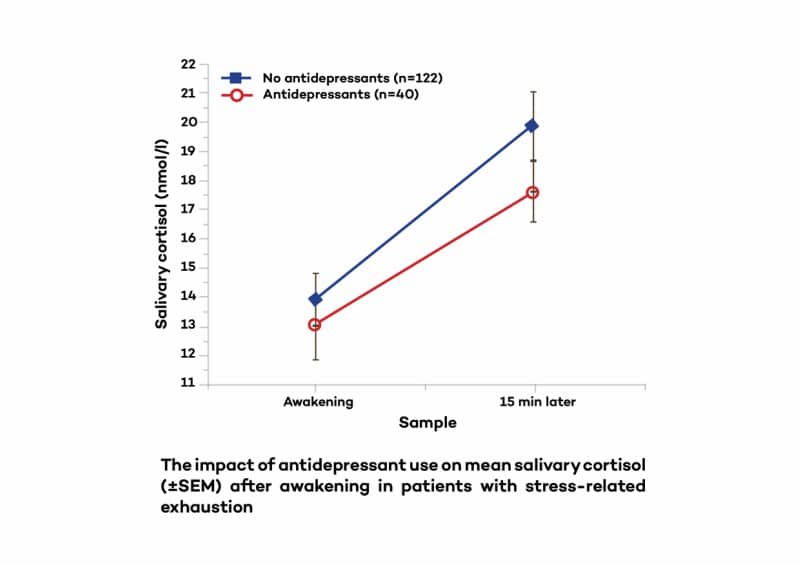
Again, both groups had stress related exhaustion, but only the group on antidepressants had the low morning cortisol awakening response.
So is the cortisol pattern the result of “adrenal fatigue” or simply taking antidepressants?
5. Being sedentary
Several studies have shown that being sedentary can cause a lower morning peak in cortisol levels.[34]
Here is one study that looked at people with major depression to examine how their physical activity habits related to their cortisol patterns.
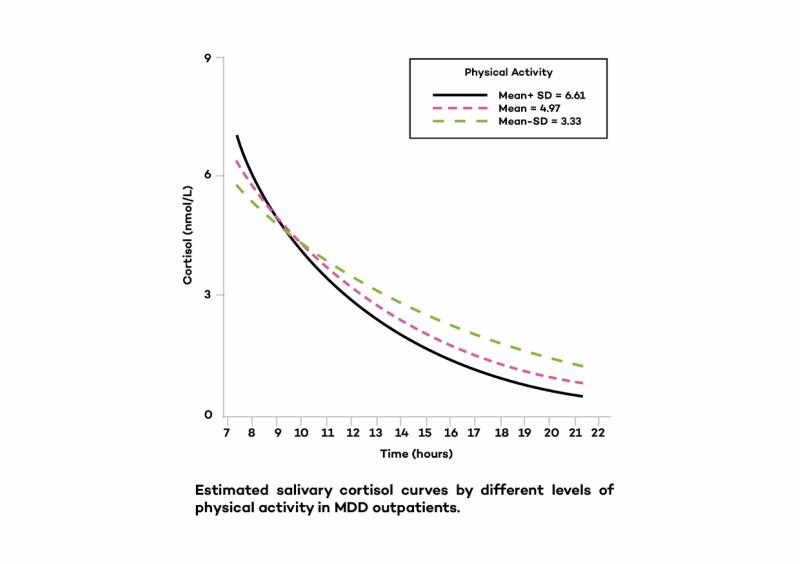
Higher physical activity led to a more pronounced rise (awakening response) and fall of daily cortisol levels.
6. Having a day off work instead of working
Research has even shown that morning cortisol awakening response can be high one day and low the next, as a simple function of whether or not someone has work that day or it’s a weekend.
Specifically, having work (and thus a greater anticipated demand of the day) will lead to a higher cortisol peak, and having a day off work leads to a lower cortisol peak.[35]
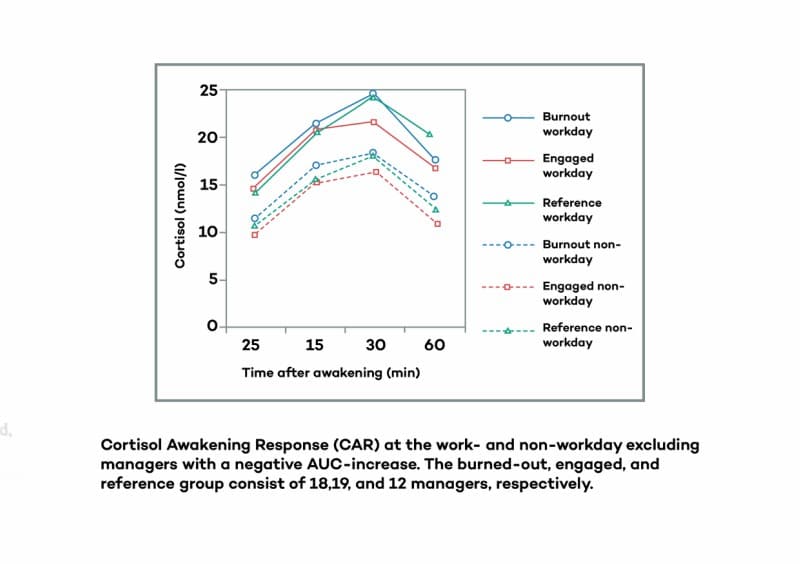
As you can see from the above graph, simply having a day off lowered morning cortisol awakening response in all groups.
Importantly, this change occurred from one day to the next, and thus contradicts the notion that it’s chronic stress that causes this lower morning cortisol pattern.
Side note: This also represents a significant confounding variable in cortisol testing, for two reasons:
- If people doing at-home tests take measurements on non-work days, they measure lower than on other days.
- Patients in chronic fatigue groups likely have more non-working persons compared to healthy people. So the studies comparing chronic fatigue patients to healthy people are confounded by the fact that many people with chronic fatigue will have cortisol patterns that reflect non work days.
So is it “adrenal fatigue” or simply a reflection of the perceived demands of the day?
7. Poor sleep (or lack of sleep)
This is likely the biggest factor of all.
Several studies have shown that simply sleeping poorly will cause a lower peak in morning cortisol.[36] [37]
There is no need for chronic stress to exhaust the adrenals – a single night of poor sleep will cause the same exact cortisol abnormality that some people claim to be the “cause” of chronic fatigue.
Moreover, it is known that people who develop chronic fatigue syndrome often develop sleep problems. Thus, the sleep problems that emerge in many people with chronic fatigue may actually be the biggest factor in causing the low peak in morning cortisol in some people.
Here’s where this gets particularly interesting. There is research showing that people with chronic fatigue syndrome have unusually high rates of sleep disorders. For example:
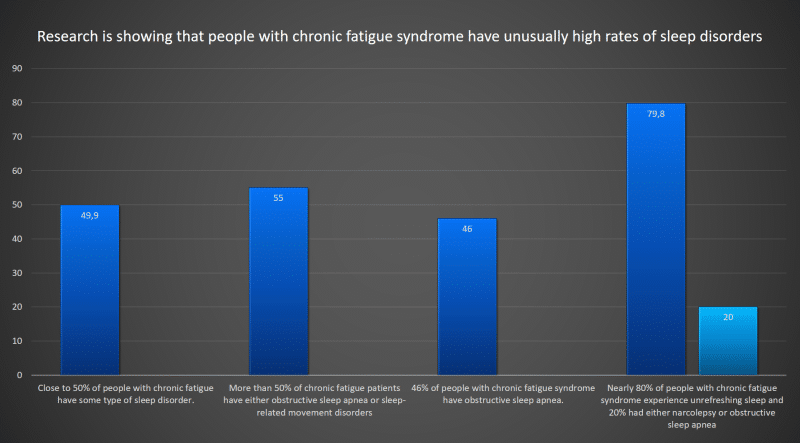
- Studies have shown that close to 50% of people with chronic fatigue have some type of sleep disorder.[38]
- One study found that more than 50% of chronic fatigue patients have either obstructive sleep apnea or sleep-related movement disorders (e.g. restless leg syndrome).[39]
- Another study found that a whopping 46% of people with chronic fatigue syndrome have obstructive sleep apnea.[40]
- Another large, population study showed that nearly 80% of people with chronic fatigue syndrome experience unrefreshing sleep and 20% had either narcolepsy or obstructive sleep apnea.[41]
When you consider how common poor sleep and full blown sleep disorders are in chronic fatigue syndrome – and when you consider that sleep problems alone will cause low morning cortisol levels – it’s actually a wonder that so most studies still show that most people with chronic fatigue have perfectly normal cortisol levels!
In short, the fact that poor sleep itself causes low morning cortisol, and the fact that poor sleep is so common in people with chronic fatigue strongly suggests the possibility that the lower cortisol isn’t causing the whole condition, but that low cortisol is simply an epiphenomenon – an effect of one of the symptoms of chronic fatigue: disrupted sleep.
Moreover, in case you would still be inclined to try to explain things through the lens of “adrenal fatigue” theory and say that the poor sleep is exhausting the adrenals, it’s worthwhile to note that the research has actually shown that even a single night of poor sleep will cause low morning cortisol, and that simply correcting the sleep can immediately resolve the cortisol pattern back to normal, within just days.[42] In other words, there is no need to invoke any theories about the adrenals getting “fatigued” in order to explain a low peak in morning cortisol – it may simply be an acute response to poor sleep. There is research that supports this:
“Both daily variations in sleep behaviors and ongoing sleep disturbance and fatigue are associated with a disrupted cortisol rhythm. In contrast, prior-day napping is associated with a more robust cortisol rhythm.”[43]
In other words, the morning peak in cortisol levels changes from one day to the next according to how much sleep you get. Sleep more and take a nap in the afternoon and you can bring your morning cortisol levels back up to normal the next day.
Another study in people with depression supports this view as well. They found that it is only those people who have trouble sleeping that have low morning cortisol – i.e. the people with depression who don’t have sleep problems have normal cortisol levels.[44] Again, this suggests that it is the sleep issues that are causing the cortisol abnormalities. (I.e. The low morning cortisol isn’t the “cause” of the depression – it’s simply an epiphenomenon that occurs in those depressed people who don’t sleep well.)
One study on people with burnout syndrome went so far as to say
“The data supports the notion that sleep impairments are causative and maintaining factors for this condition.”[45]
Another study in chronic fatigue syndrome concluded:
“Neuroendocrine abnormalities (i.e. low morning cortisol) reported to be characteristic of chronic fatigue syndrome may be merely the consequence of disrupted sleep and social routine.”[46]
The simple fact is that this one factor – poor sleep – is, by itself, enough to explain why a subset of people with chronic fatigue have low morning cortisol levels.
To sum up:
It is known in the research that people who are night owls and/or poor sleepers have higher rates of burnout/chronic fatigue. So we know that if we compare a group of people with chronic fatigue/burnout to a group of normal healthy people, it is virtually guaranteed that the chronic fatigue/burnout group will have more night owls and/or poor sleepers (i.e. people with insomnia).
(And it is also extremely likely that the chronic fatigue/burnout groups will have higher rates of the other factors, like antidepressant use, lower physically activity, and excess body fat compared to the general healthy population).
Here’s the key point: Simply because the chronic fatigue/burnout group of people will likely have more individuals that have these factors going on – i.e. they are poor sleepers, night owls, sedentary, on antidepressants, or are overweight – these studies are very likely to conclude that overall, people with chronic fatigue/burnout have lower morning cortisol levels. (Since the people with these factors will skew the overall average cortisol numbers of the entire group).
Considering how common poor sleep is in people with chronic fatigue, it is actually shocking that most studies still find perfectly normal cortisol levels in the vast majority of people with chronic fatigue/burnout.
Indeed, the fact that so many common lifestyle factors (that are known to be especially common in people with chronic fatigue) can induce low morning cortisol levels, and yet, the majority of studies still find normal cortisol levels in most people with chronic fatigue adds further evidence to the notion that cortisol levels are simply not a significant causal factor in chronic fatigue.
The point here is to simply say that the proposed cortisol abnormality claimed to be associated with fatigue/burnout (lower morning peak in cortisol) it not actually not unique to fatigue/burnout – it arises all the time in people without fatigue/burnout. Nor is it evidence of “adrenal exhaustion” due to chronic stress – the same cortisol pattern arises in people all the time without any chronic stress over months or years taxing their adrenals.
Low morning cortisol levels do not mean that the adrenals have been exhausted and can’t produce enough cortisol – it is often an acute hormonal response to simply being a night owl, being overweight, being a night eater, being on antidepressants, or not sleeping well. It doesn’t even require months or years of these factors – it can arise from simply staying up late the night before, or poor sleep the night before. One can even have a lower morning cortisol peak from simply having a day off of work.
In short, low morning cortisol levels are not evidence of exhausted adrenal glands, but may simply be an acute hormonal response to being a night owl, medication use, night eating, being overweight, or poor sleep.
Making Sense of The Science: When Cortisol Levels Are Low (in a Minority of People with Chronic Fatigue), it’s Likely a Consequence (or Epiphenomenon), Rather than a Cause of Chronic Fatigue
We now know 4 important facts about the cortisol patterns seen in people with chronic fatigue/burnout:
- Low morning cortisol levels are not present in the majority of people with chronic fatigue/burnout.
- Low morning cortisol levels are not present at the onset or early stages of chronic fatigue/burnout.
- Raising cortisol levels (via medication) does not resolve the fatigue or provide any meaningful benefit over a placebo for the vast majority of people with chronic fatigue. (Including those with measurably low cortisol).
- Low morning cortisol levels can be caused by simply being a night owl, taking antidepressants, being sedentary, being overweight, or not sleeping well. (Thus lower morning cortisol levels in some people are easily explained by just those people who are poor sleepers.)
Taken together, these facts make it clear that that abnormal cortisol/HPA axis function is not a primary cause of chronic fatigue.
The cortisol abnormalities that do occur in a subset of people with chronic fatigue can also be easily explained. These abnormalities may simply be a consequence of some of these lifestyle and behavioral factors, rather than a cause of the whole condition of chronic fatigue/burnout.
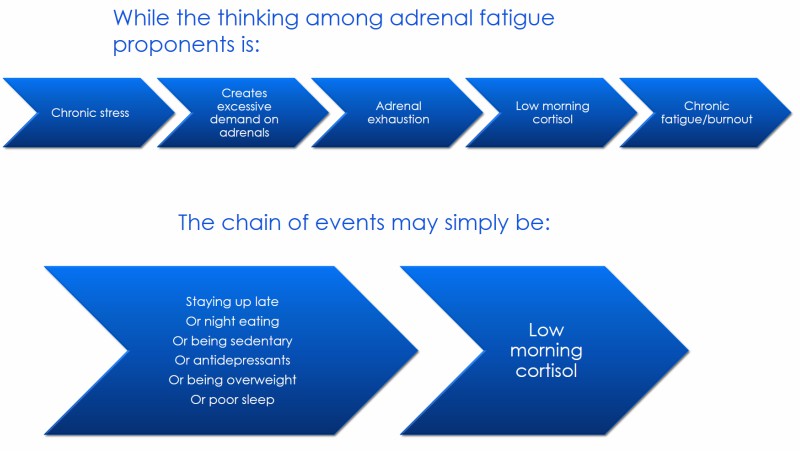
And this is why many researchers have concluded that HPA axis dysfunction and cortisol abnormalities are likely not a major cause of chronic fatigue/burnout, but arise as an effect of some of the lifestyle factors (e.g. insomnia, lack of physical activity, medication use, etc.) that commonly occur in chronic fatigue/burnout.
And this is precisely what one of the biggest reviews of the scientific research, The HPA axis and the genesis of chronic fatigue syndrome, concluded:
“A reversed direction of causation (i.e. that the illness leads to HPA axis changes rather than the other way around) is supported by the findings that there is an apparent absence of HPA axis changes early in the genesis of chronic fatigue states, and that modifying cognitive behavioural components of the illness leads to a normalization of the HPA axis.”[58]
Another very recent systematic review of the science from 2013, titled A Review of Hypothalamic-Pituitary-Adrenal Axis Function in Chronic Fatigue Syndrome stated:
“the abnormalities (in HPA function) are subtle, and there is marked variation in basal and challenge tests in CFS patients and a real risk that these so-called abnormalities are simply confounds or epiphenomena.”
Another study concluded:
“Few studies report on severity of the fatigue or disability, and there is reason to suggest that some behavioural consequences of fatigue may themselves cause the shift in adrenocortical functioning … For example Leese et al. found that short-term night-shift working mimics the HPA changes observed in patients with CFS. They conclude that the changes observed in CFS may be secondary to disrupted sleep and social routine, and thus an epiphenomenon in terms of fatigue causation.”[59]
One of these systematic literature reviews concluded:
“Inactivity, sleep disturbance, psychiatric comorbidity, medication, and ongoing stress experienced by people with CFS will affect HPA axis function, and the findings that HPA axis dysregulation is more prominent in patients with a longer duration of illness suggest that the endocrine changes may be secondary.”[60]
One study on burnout went so far as to say:
“The data supports the notion that sleep impairments are causative and maintaining factors for this condition.”[61]
Another study concluded:
“Neuroendocrine abnormalities (i.e. lower morning cortisol) reported to be characteristic of chronic fatigue syndrome may be merely the consequence of disrupted sleep and social routine.”[62]
So are lower morning cortisol levels in a subset of people with chronic fatigue evidence that adrenal fatigue is real? No.
While some people believe that a low morning cortisol peak means that a person has “adrenal fatigue,” it may actually just mean that a person has excess body fat, or is sedentary, or is taking medications, or is a poor sleeper, or stays up late (or a combination of those factors).
The simple facts presented above can easily explain why a subset of people with chronic fatigue/burnout have a smaller morning peak in cortisol levels.
Based on this research, what can we say about the question “is adrenal fatigue real?”
Since cortisol abnormalities are not typically present at the onset or early stages of chronic fatigue, and since cortisol abnormalities are not present at all in the vast majority of people with chronic fatigue, a reversed direction of causation – where cortisol abnormalities are caused by other factors, inactivity, medication use, poor sleep, etc. – is the most compelling explanation for cortisol abnormalities, in the minority of people with chronic fatigue who do have them.
More Problems With Adrenal Fatigue
There are also a number of other problems with the theory of “adrenal fatigue” and the way it is diagnosed and treated. In this section, we will address some of these issues that further question the scientific validity of the diagnosis and treatment of “adrenal fatigue.”
(In an effort to keep things organized and easy to understand, we’ve put the following sections in the pop-out boxes below. Please click the boxes below to unveil text for each of the below topics).
Inaccuracy of Cortisol Tests
Interestingly enough, most people who are diagnosed with low cortisol and “adrenal fatigue” or “adrenal exhaustion” don’t actually have low cortisol levels. There are several serious methodological problems in the way cortisol levels are often tested that lead to faulty results.
There are 4 reasons why this happens:
1. Tests that don’t give the full picture of cortisol amounts.
See, there are different ways of measuring cortisol.
- Saliva
- Blood (serum)
- Hair
- Urine
The practitioners who believe in adrenal fatigue have generally relied on saliva measurements (also called the Adrenal Stress Index). Saliva measurements of cortisol are indeed a valid method of assessing free cortisol. But, it’s important to understand what is actually being measured. Saliva measurements measure unbound or “free” cortisol – i.e. cortisol not bound to a protein carrier molecule. This is only about 3-5% of total cortisol in our body at any moment. The rest of the cortisol may be bound or in some step of the metabolic pathways involved in clearance of cortisol through the urine. So saliva cortisol doesn’t really give the whole picture about total cortisol produced by the adrenal glands.
The claim in “adrenal fatigue” is that the adrenals get worn out and can’t produce enough cortisol. Yet, saliva measurements do not allow us to assess the amount of cortisol produced by the adrenals – only the amount of cortisol that is free cortisol in the body at a given time.
The ideal marker of total cortisol production in the body is measuring cortisol metabolites (breakdown products) in the urine, because that reflects the other 95-97% of cortisol that our body produces.
Why does this distinction matter?
Simple: Because research has now found that many people who have low cortisol based on saliva tests (and who are told that their adrenals are exhausted and can’t produce enough cortisol) actually show normal or even high total cortisol production.
(Note: This pattern of low free cortisol but high total cortisol is actually extremely common — particularly in overweight people, which the majority of people in the Western world now are. So this scenario of low cortisol in saliva testing, but high total cortisol production is actually extraordinarily commonplace – to the point where most people who are told they have low cortisol levels based on saliva tests don’t actually have low cortisol.)
Want to know just how common this is? Here’s functional medicine practitioner Chris Kresser explaining it in more detail:
“According to unpublished data from a lab called Precision Analytical that does cortisol testing, of 2,000 test subjects that they’ve looked at with low free cortisol, only 15% actually had low total cortisol. So, put [in] a different way, people with low free cortisol were actually more likely to have normal or high total cortisol than they were to have low total cortisol.”[64]
This is clearly a big problem. Why? Consider that many practitioners prescribe external cortisol (hydrocortisone) to people that they diagnose with low cortisol.
In this scenario, a person might even be told that their cortisol is low, and then put on glucocorticoid medication or other substances to try to raise cortisol, not realizing that cortisol is already too high. This obviously has the potential to make a person worse.
Again, it’s worth emphasizing this because it’s so shocking: It is actually more common for a person with low cortisol on saliva tests to have normal or high total cortisol production, than to actually have low cortisol.
2. Tests administered only once.
This is a fairly straightforward one. Many practitioners only do a single saliva test. This is simply not accurate. Cortisol levels fluctuate dramatically over the course of 24 hours. They even fluctuate dramatically within the span of a single hour, in the first hour after awakening (called Cortisol Awakening Response). So these single measurement tests simply are not accurate measures of anything.
To get reliable and accurate measurement of cortisol, one should ideally do multiple saliva tests over the course of 24 hours. Or at least, multiple time points within the first hour after awakening to assess the cortisol awakening response.
3. Some functional medicine labs have revised their “reference ranges” in a very narrow range.
The “reference range” is the range of cortisol values that a lab uses to interpret lab results and say what is considered normal, or abnormal.
What this means is that by having a narrow reference range, more people will fall outside of the normal and thus will be diagnosed with low cortisol.
Many labs have changed the reference ranges in recent years, and these revisions are generally not supported by endocrinologists or based on sound scientific evidence.
In other words, some independent labs and individual practitioners simply choose to arbitrarily decide what they believe should be the “normal cortisol” values, and then create a very narrow range for it (much more narrow than conventional endocrinologists) and thus, many more people are diagnosed with abnormally low cortisol levels.
4. Tests are often not administered at the correct time in the morning
Another massive problem with cortisol testing is that because of the huge change in cortisol levels in the first hour after awakening, taking the measurement 30 minutes or 60 minutes later than one was supposed to take it can give a reading that is dramatically lower than the actual cortisol levels.
As soon as we wake up in the morning and light enters our eyes, it initially a steep and dramatic rise in cortisol levels within the first 15 to 30 minutes after awakening. This is called the “Cortisol Awakening Response.” (This steep peak in cortisol levels accounts for over 50% of our total cortisol production during each 24 hour day.) Importantly, after the initial hour after awakening, there is a massive and rapid decline in cortisol levels.
To show you what I mean, take a look at this image of the cortisol awakening response.
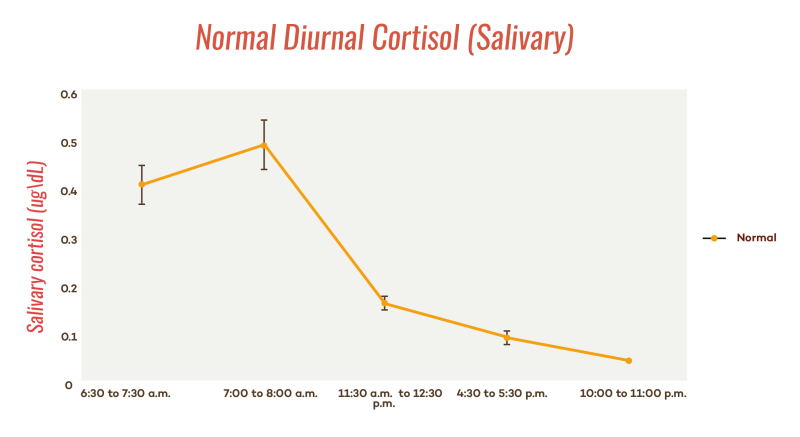
Do you notice how much cortisol values change in just 30 minutes or an hour?
So what would happen if the test is administered just one hour or two hours later than it’s supposed to be?
You’d obviously get a wildly inaccurate cortisol level.
It turns out that this is exactly what has happened on a massive scale. Many of the labs doing these cortisol tests didn’t instruct people to take their first saliva sample within the first 30 minutes of after awakening.
So what this amounts to is that tens of thousands of people who have had cortisol testing for “adrenal fatigue” took their first saliva samples an hour or two hours into the morning, which misses the entire cortisol awakening response and gives a completely inaccurate cortisol reading. Specifically, it will give a much lower cortisol level than is actually the real amount of cortisol your body makes in the morning.
I can’t emphasize enough how big of a blunder this is. Accurate cortisol readings depend on the saliva sample being taken in the first 30 minutes after awakening. If you take your morning sample an hour or two after waking up, it is virtually guaranteed to get someone falsely diagnosed with low cortisol.
Based on the above factors, what can we say about the question “is adrenal fatigue real?”
It is likely that a sizable portion of people being diagnosed with low cortisol levels and “adrenal fatigue” actually have perfectly normal adrenal function and cortisol levels.
The Real Symptoms of Low Cortisol Don't Match Up With The Claimed Symptoms of "Adrenal Fatigue"
One of the most glaring problems with the “adrenal fatigue” theory is that the claimed symptoms (of adrenal fatigue) do not actually match up with the actual symptoms that are accepted to be associated with low cortisol.
Here are the symptoms claimed to be caused by “adrenal fatigue”:

- Fatigue and lack of energy
- Weight gain (especially “belly fat”)
- Depression
- Anxiety
- Brain fog
- Low blood sugar
- Low libido
- Waking up tired even after sleeping 7 or 8 hours
- Cravings for sugary and salty foods
- Trouble sleeping through the night (especially waking up between 2-4am)
And here are the symptoms that are actually caused by low cortisol levels:

- Fatigue
- Weight loss
- Low appetite or anorexia
- Darkening of your skin (hyperpigmentation)
- Low blood pressure, even fainting
- Salt craving
- Low blood sugar (hypoglycemia)
- Nausea, diarrhea or vomiting
- Abdominal pain
- Muscle or joint pains
- Irritability
- Depression
- Body hair loss or sexual dysfunction in women
You’ll notice that there are some of the symptoms on both lists – like fatigue, low blood sugar, depression, and cravings for salt.
But there are also several major discrepancies – it’s actually weight loss (not weight gain) that is associated with low cortisol, as well as things like nausea, diarrhea, vomiting, abdominal pain, muscle/joint pains, body hair loss, skin darkening, and loss of appetite (the opposite of sugary food cravings) that are all common symptoms of low cortisol that are not claimed to be associated with “adrenal fatigue.”
In addition, it’s also worth pointing out that the symptoms claimed for “adrenal fatigue” are significantly more common occurrences in regular healthy people, and are not specific to low cortisol states or people with chronic fatigue issues, such as weight gain, cravings for sugary foods, anxiety, waking up tired, and trouble sleeping. These are all symptoms that apply to large portions of the general population, and are not unique to people with chronic fatigue or low cortisol. Thus, a huge percentage of the general healthy population will identify with these symptoms.
In fact, if you go to chiropractor and naturopath James Wilson, D.C.’s (the creator of “adrenal fatigue”) website, www.adrenalfatigue.org and take his symptoms-based quiz that supposedly helps determine if you have adrenal fatigue, here is his initial list of symptoms:

- Tired for no reason?
- Having trouble getting up in the morning?
- Need coffee, cola, salty or sweet snacks to keep going?
- Feeling run down and stressed?
- Crave salty or sweet snacks?
- Struggling to keep up with life’s daily demands?
- Can’t bounce back from stress or illness?
- Not having fun anymore?
- Decreased sex drive?
If you answered yes to even a few of these questions, he claims that this means you may have adrenal fatigue.
Now look over that list closely. Do you anyone who wouldn’t at least say yes to at least a few of those questions, at least some of the time?!
What I am suggesting is that he has coined a new syndrome (“adrenal fatigue”)…
then created a diagnostic criteria of adrenal fatigue where no matter whether a person has high, normal or low cortisol they may still be diagnosed with adrenal fatigue…
and then created a very broad list of general symptoms that even a large percentage of healthy people will identify with.
So I decided to do a survey to get to the bottom of this discrepancy between the actual symptoms of low cortisol levels vs. the claimed symptoms of adrenal fatigue.
I wanted to know if a population of people with fatigue – most of whom were convinced that they had “adrenal fatigue”(or have officially been diagnosed with it) – would actually identify with the real symptoms of low cortisol levels.
I took a sample of over 600 people with fatigue and then simply presented them with the actual symptoms that are associated with low cortisol (see the list above).
Then I simply told them
“Can I ask for your help with this little survey? It’s a list of 12 symptoms, and I just want to know whether this list of symptoms feels like a good fit with YOUR symptoms, or if it doesn’t seem like a very good fit.
In other words…
Do you read this list of symptoms and think “Wow, that sounds like what I have” or “No, that doesn’t really sound like what I have.”
Please only say “Yes, this sounds like what I have” if you identify with at least 6 of the 12 symptoms.
Otherwise, say “No, this doesn’t really sound like it matches well with my symptoms”
Here is what I was covertly doing…
Again, the list of symptoms I posted are the actual symptoms of low cortisol levels. (Not the much different, much more vague and general, list of symptoms claimed for “adrenal fatigue.”)
This simple survey was designed to find out if people with fatigue (many or most of whom believe they have adrenal fatigue) would actually identify with the real symptoms of low cortisol levels.
Here are the results:
- 77 of 621 people (12.4%) of people said that the symptoms of low cortisol are very similar to their symptoms.
- 544 of 621 people (87.6%) of people said that the symptoms of low cortisol are not similar to their symptoms.
Well, simply put, it means that the vast majority of people with fatigue do not have the symptoms associated with low cortisol levels. Over 8 out of 10 people with fatigue do not identify with the symptoms of low cortisol levels.
This is just one more piece of data to go along with dozens of actual scientific studies on this subject again suggesting that the vast majority of people with chronic fatigue do not actually have low cortisol levels.
Based on this research, what can we say about the question “is adrenal fatigue real?”
- If most people with fatigue don’t have symptoms of low cortisol, it doesn’t make much sense to attempt to explain chronic fatigue by saying that it’s caused by low cortisol.
- This is particularly true in light of the fact that we have already seen from the actual studies that most people with chronic fatigue do not actually have abnormal cortisol levels.
- If studies don’t show low cortisol levels in the majority of people with chronic fatigue, and most people with chronic fatigue don’t identify with the symptoms of low cortisol levels, it simply does not make sense to keep focusing on cortisol as a valid way of explaining fatigue.
Many Different Cortisol Abnormalities (and Even No Abnormality At All) Can All Still Get You Diagnosed With "Adrenal Fatigue"
Another problem with the “adrenal fatigue” theory is the rules (or lack of rules) many people are using to interpret cortisol tests.
As you’ve now seen, cortisol levels are an extraordinarily bad predictor of whether or not someone is fatigued. A person who is completely exhausted and burned out from chronic stress may have high cortisol, or low cortisol or normal cortisol. As explained above, in the setting of any illness, this scenario should immediately get that biomarker ruled out as an invalid way of diagnosing a condition. Yet, many health practitioners still claim to diagnose “adrenal fatigue” based on cortisol measurements.
The interesting thing that many people have done though, is basically rigged the game to virtually always come out with an adrenal fatigue diagnosis.

- If a person has high cortisol, they may be told they’re in the “first stage of adrenal fatigue.”
- If they have normal cortisol levels, they may be told they’re in an early stage or middle stage, before their cortisol levels decline.
- If they have low cortisol, they may be told they’re in a “late stage of adrenal fatigue.”
In other words, they’re using a diagnostic marker that can potentially always be used to claim that someone has “adrenal fatigue” – regardless of whether cortisol is high, low, or totally normal.
(It’s important to note here that these supposed “phases” of “adrenal fatigue” are not validated by scientific research. Indeed, as we’ve seen in the research, cortisol levels do not have any reliable relationship to the severity of chronic fatigue).
Again, in conventional medicine, in any scenario like this, this way of diagnosing people with a condition would immediately be recognized as scientifically invalid. A biomarker that is this inconsistently associated with a set of symptoms would immediately be thrown out as an invalid biomarker for that condition.
The Treatments Typically Given To People Diagnosed with "Adrenal Fatigue" Don't Actually Raise Cortisol Levels
This is another area where the adrenal fatigue theory just doesn’t make sense. The claim with adrenal fatigue is that the adrenals get burned out and then low cortisol levels produce fatigue and many other symptoms.
Key point: The primary claim of adrenal fatigue is that it’s low cortisol levels in people with “adrenal fatigue.”
Here’s why that’s a critical point to pay attention to: The supplements typically prescribed by alternative health practitioners to correct adrenal health don’t have scientific evidence showing that they raise cortisol levels.
In fact, virtually all the evidence on virtually all of the supplements prescribed to people with “adrenal fatigue” have actually been shown in the research to lower cortisol levels!
Obviously if the claim is that someone has low cortisol levels, it doesn’t make sense to prescribe things which are known to lower cortisol levels.
Here are some of the most typical substances prescribed to people with “adrenal fatigue”:

- Rhodiola rosea
- Ashwagandha
- Lemon balm
- Licorice root
- Phosphatidylserine
- Ginseng
- Tulsi
The lone exception that works to potentially raise cortisol levels (by inhibiting cortisol conversion to cortisone) is licorice root.
For all the other herbs and supplements commonly prescribed to people with low cortisol levels, the scientific evidence only shows that these substances lower cortisol levels!
I am not aware of any studies that have ever shown that any of these substances work to increase cortisol.
And in speaking with functional medicine and adrenal function expert, Dr. Bryan Walsh, he said “I have literally never seen adaptogenic herbs raise cortisol levels.”
If the claim is that people with “adrenal fatigue” have symptoms due to low cortisol levels, it does not make sense to prescribe substances that are proven to lower – not raise – cortisol levels.
Moreover, it also does not make sense to explain the benefits of these substances (which are real) through the lens of how they affect cortisol levels. (In reality, they affect many other systems of the body, including the brain, the immune system, inflammatory cytokines, and perhaps most importantly, the mitochondria (the energy generators in our cells)).
How does all of this relate to the question “is adrenal fatigue real?”
To sum up: If low cortisol is the problem, it doesn’t make sense to prescribe substances that are proven to lower cortisol levels.
Most Studies Attempting to Link Cortisol Levels with Various Illnesses and Symptoms (e.g. Chronic Fatigue/Burnout) Have Major Confounding Variables That Are Not Controlled For in The Research
As you saw in the previous section, it is now known that many physical traits and behaviors can induce cortisol abnormalities. Indeed, there are actually many more factors than just what I mentioned above that influence the daily cortisol pattern:

- Body fat
- Physical activity
- Medication use (e.g. antidepressants, anti-anxiety meds, painkillers, opioids, stimulants, etc.)
- Chronotype (night owls vs. morning types)
- Eating habits (e.g. night eating)
- Psychological traits (e.g. loneliness)
- Genetics
- Perceived overall stress load
- Perception of upcoming stress of the day (e.g. workdays vs. non-workdays)
- Psychiatric illness (e.g. depression, anxiety disorders, schizophrenia, PTSD)
- Poor sleep
Importantly, the studies assessing cortisol levels in various illnesses have almost universally failed to control for most or all of these variables.
Thus the claims of how cortisol abnormalities are linked with various illnesses should be taken with a grain of salt.
These are all major confounding variables in the studies which have tried to link abnormal cortisol patterns to various diseases (including chronic fatigue/burnout).
What this means is that many of the supposed cortisol abnormalities in such diseases may simply be effects of symptoms of the disease (e.g. taking painkillers, poor sleep, or being physically inactive due to fatigue), rather than actual causes of the disease. Or they may simply be due to co-occurrences – for example, insomnia, depression, and excess body fat are all common co-occurrences in numerous different diseases.
In other words, while the common thinking of adrenal fatigue proponents is to point to cortisol abnormalities as a causal factor in the disease, there is much research indicating that it may be a reversed direction of causation – that these symptoms and lifestyle factors (e.g. poor sleep, excess body fat, medication use, etc.) are causing the abnormal cortisol patterns, rather than the other way around.
It’s also important to recognize that a lower morning peak in cortisol can be caused by numerous different lifestyle variables that change on a day to day basis, and are not valid evidence of “exhausted adrenal glands.”
Moreover, I have literally never heard any health practitioner even mention these confounding factors when they analyze cortisol results of individuals they are working with.
To give just one example of why this is problematic: Let’s take a person who has low morning cortisol levels and their doctor believes that it’s due to “exhausted adrenals.” In reality, it may simply be due to the fact that the person is a night owl and they typically go to bed very late and don’t sleep enough. Instead of addressing the person’s sleep hygiene habits, the doctor may prescribe hydrocortisone to treat the low cortisol levels. Of course, this mistake in treatment approach – treating the cortisol levels instead of treating the sleep habits – may have major health consequences over time.
As one 2017 review of the science on cortisol patterns in disease stated:
“Given that the bulk of the research examined was cross-sectional in nature, it is possible that a flattened DCS (diurnal cortisol slope, or pattern with a lower morning peak in cortisol) is a symptom, or a consequence, of a prior disease state. Many diseases result in physical pain and psychological stress. Consequently, a flattened DCS could be caused by pathophysiological or stress-related changes resulting from the experience of the disease itself. …Together, these findings suggest a reverse-causal explanation deserves more attention in future research.”[65]
Of course, it is still possible and likely that truly low cortisol levels may be a causal or perpetuating factor in some illnesses. The researchers of the 2017 literature review concluded that the effects likely go both ways:
“Given the transactional nature of the regulation of interrelated biological systems, and our findings of associations between flatter DCS (lower morning peak in cortisol and/or higher even cortisol levels) and multiple health outcomes, it seems plausible that reciprocal and cascading interactions among clock gene mechanisms, sleep, cortisol, inflammation, fatigue, appetite, behavior, and social and psychological experiences jointly contribute to the observed associations between flatter DCS and multiple types of negative health outcomes.”[66]
In short, while cortisol abnormalities may be a contributing factor in some conditions, the evidence being used to claim them as a causal factor is weak, and confounded by over a dozen variables.
In the case of chronic fatigue, we should be very cautious with assuming that a low morning cortisol peak is valid evidence of any sort of “adrenal fatigue.” As discussed above, low morning cortisol levels may simply be an indication of a sedentary lifestyle, excess body fat, poor sleep, night eating, disrupted circadian rhythm, taking certain prescription or over-the-counter drugs, or simply staying up late.
Moreover, we must remember that the research isn’t even consistent in showing any specific type of cortisol or HPA abnormality in relation to fatigue. As one review of the research put it:
“The above cited literature shows that the evidence on possible relationships between burnout and vital exhaustion on the one hand and HPA axis (dys)regulation on the other remain somewhat inconsistent. For example, there are studies showing either lower, higher or unchanged cortisol awakening profiles in groups with higher levels of burnout. … even some very well-conducted studies could not find associations between burnout and HPA axis dysregulations.”[67]
Based on this research, what can we say about the question “is adrenal fatigue real?”
Virtually all of the research done trying to link cortisol levels with chronic fatigue (and most others diseases) is cross-sectional and thus, confounded by multiple factors that influence cortisol levels. So one should take such studies skeptically.
As discussed above, in chronic fatigue/burnout, the case for a reversed direction of causation – i.e. the illness and behavioral consequences of it, cause cortisol abnormalities in some subset of patients – is more compelling than the case for cortisol abnormalities being a significant causal factor.
Is Adrenal Fatigue Real – Summary
In summary, the scientific evidence does not support the notion that adrenal function/HPA axis function/cortisol are a significant causal factor in chronic fatigue.
Here is the bullet-point summary of the key points in this article:
- The “adrenal fatigue” theory is not supported by the research.
- Studies have been conducted by researchers all over the world for over two decades examining whether adrenal/HPA axis dysfunction is a primary cause of chronic fatigue/burnout. 20 years of research into this has failed to show any type of HPA or cortisol abnormality that is reliably found in people with chronic fatigue/burnout.
- Overall, the research indicates that the majority of people with chronic fatigue/burnout have normal cortisol levels. Thus cortisol levels cannot reasonably be said to be the “cause” of chronic fatigue if it’s not even detectable in the majority of people with chronic fatigue.
- The research shows no clear link between cortisol levels and chronic fatigue/fibromyalgia/burnout. Some studies indicate increased cortisol in people with chronic fatigue/burnout, others show decreased cortisol, and the vast majority of studies show no differences in cortisol levels at all.
- Cortisol levels are not a valid biomarker of fatigue or burnout. If poor adrenal function/low cortisol were the primary cause (or even a major cause) of chronic fatigue/burnout, we would expect to find that all (or at least a large majority of) people with chronic fatigue/burnout have low cortisol levels. Yet, the vast majority of people with chronic fatigue or burnout from stress have no cortisol abnormalities at all. Thus cortisol levels are not a valid biomarker of chronic fatigue.
- Cortisol levels measurements are not a valid way of diagnosing people with chronic fatigue/fibromyalgia/burnout vs. normal healthy people. There is no specific cortisol/HPA abnormality seen in these conditions, and no abnormality at all in most people. A small subset of people (likely between 15%-25%) with chronic fatigue/burnout have a lower morning peak in cortisol levels. (This lower morning peak in cortisol occurs as a result of many common variables – including being overweight or simple lack of sleep – and is not unique to chronic fatigue/burnout). There is no evidence to suggest that this low peak in morning cortisol is a causal factor, since it is not present at all in the majority of people with chronic fatigue/burnout.
- Even studies that do find cortisol abnormalities show only very slight abnormalities — and typically still show normal overall 24-hour cortisol output. Thus, there appears to be little to no evidence suggesting that the adrenals are incapable of producing enough cortisol.
- Low salivary cortisol levels are not actually evidence of “adrenal fatigue.” Research that assessing total 24-hour cortisol output via urine shows that the majority of people who have low salivary cortisol levels actually have normal total 24-hour cortisol production by the adrenal glands.
- There are no cortisol abnormalities present at the onset or early stages of chronic fatigue. If poor adrenal function/low cortisol levels were a cause of chronic fatigue/burnout, we should expect to find low cortisol levels at the onset or early stages of these conditions. Yet, we do not find that. Thus poor adrenal function or low cortisol levels cannot reasonably be said to be a “cause” of chronic fatigue.
- Cortisol level measurements are not a valid way of assessing the severity of chronic fatigue. If cortisol levels were a major cause or contributor to chronic fatigue, we would expect to see a reliable relationship where the more severe the symptoms are, the larger the cortisol abnormality we would expect to find. Yet the research shows that cortisol levels are not a valid predictor of symptoms, and do not typically relate to symptom severity.
- Cortisol level measurements are not a valid way of assessing the cause of chronic fatigue. Cortisol level testing is useful for ruling out legitimate medical conditions like Addison’s disease and Cushing’s disease, but appears to be of little to no value in chronic fatigue/burnout.
- Cortisol level measurements are not a valid way of directing the course of treatment for chronic fatigue. Measuring cortisol levels to detect cortisol abnormalities is of little value in helping people with chronic fatigue, since treatments that target directly increasing cortisol levels have largely proven ineffective.
- Cortisol testing has many methodological flaws that can often lead to false diagnoses of low cortisol levels when a person doesn’t actually have low cortisol levels.
- The notion of “phases” of adrenal fatigue that have clear connections to specific levels of cortisol has not been validated by science. People with severe chronic fatigue may have high, low, or perfectly normal cortisol levels.
- The adaptogenic herbs often prescribed to people who have been told they have “adrenal fatigue” are only shown in the scientific research to lower cortisol levels – not raise them. It does not make sense to prescribe substances that lower cortisol, if the claim is that chronic fatigue is being caused by cortisol levels that are already too low.
- The symptoms claimed for “adrenal fatigue” are vague and generalized symptoms that are not actually unique to low cortisol levels or chronic fatigue. (I.e. A large portion of the healthy general population will say “yes” in response to many symptoms listed on “adrenal fatigue” questionnaires found online).
- Lower cortisol levels – when they do occur in a small subset of people with fatigue – are almost certainly not the result of the adrenal glands being “fatigued” and unable to produce enough cortisol. If this was the case, we would see a pattern of high ACTH and low cortisol levels (as is seen in Addison’s disease), which indicates that the brain is calling for more cortisol to be produced but the adrenals are unable to produce enough. This hormonal pattern is not seen in chronic fatigue/burnout. Thus, the body is likely intentionally lowering cortisol levels and is producing exactly the amount it wants to be producing. (Again, this may be to allow inflammatory and immune responses to function well).
- The vast majority of people with chronic fatigue (over 85%) do not actually identify with the real symptoms of low cortisol levels.
- In the most generous scenario of giving some sort of importance to cortisol levels in chronic fatigue, in the subset of people with lowered cortisol levels, it is possible that this hormonal abnormality may be perpetuating the condition by creating additional symptoms and/or making recovery more difficult. Even this has not been validated by research, however. Moreover, the fact that raising cortisol levels (via hydrocortisone) fails to reliably give benefits – even to those with lower cortisol levels – suggests that cortisol levels are of minimal importance in chronic fatigue.
- A lowered morning peak in cortisol levels is something that arises in numerous different conditions, and is not unique to chronic fatigue/burnout.
- A lowered morning peak in cortisol levels is not evidence of “adrenal fatigue,” since it can be found in healthy, non-chronically fatigued people who are simply sleep deprived, sedentary, on certain medications, or are night owls.
- Cortisol levels typically do not change in response to interventions that improve symptoms and/or normalize health. If cortisol levels were the major causal factor of the symptoms in chronic fatigue/burnout, we would expect to see a reliable relationship where, as symptoms improve, so do cortisol levels. Yet, the majority of intervention studies that have shown significant improvement in symptoms (e.g. energy levels) typically show that there are no changes in cortisol levels that parallel these symptom improvements.
- Fixing cortisol levels does not fix the fatigue. This is even true in people with lower morning cortisol levels. If low cortisol were the fundamental cause (or even a major cause) of chronic fatigue/burnout, then raising cortisol levels would improve symptoms dramatically. (As it does in true adrenal insufficiency/Addison’s disease). Yet, raising cortisol levels (via medication) does not significantly improve symptoms when compared with placebo treatment. (And it may be harmful in the long run).
- The focus on cortisol levels in chronic fatigue/burnout appears to be extremely misguided. Cortisol level testing appears to be of little to no use in chronic fatigue/burnout – either diagnosing chronic fatigue/burnout or helping to direct a beneficial course of treatment. The following five points make it clear that the focus on cortisol is simply not warranted by the research:
- The vast majority of people with chronic fatigue or burnout from stress have no cortisol abnormalities at all.
- Cortisol abnormalities are not present at the onset or early stages of chronic fatigue.
- Based on the research, it appears likely that cortisol abnormalities (in the minority of people where they occur) may be just an epiphenomenon that results from being a night owl, taking antidepressants, inactivity, being overweight, or having sleep problems.
- The majority of intervention studies that have shown significant improvement in fatigue typically show that there are no changes in cortisol levels that parallel these symptom improvements.
- Interventions in people with chronic fatigue/burnout that directly target the cortisol abnormalities and raise cortisol levels (e.g. hydrocortisone) do not significantly improve symptoms vs. placebo.

So is “adrenal fatigue” real?
Overall, the theory of “adrenal fatigue” is not supported by the scientific evidence.
Over two decades ago, the theories of the “stress crash” or “HPA crash” “adrenal insufficiency period” or “adrenal fatigue” came into prominence, and have become the dominant way of thinking about chronic fatigue among most holisitic/alternative/integrative health practitioners. These theories hypothesized that the likely underlying cause of many diseases such as chronic fatigue syndrome or burnout syndrome was hormonal abnormalities (e.g. low cortisol levels) resulting from chronic stress wearing out the adrenals or HPA axis, and that these abnormal cortisol levels would turn out to be the cause of the symptoms seen in these conditions. The most common variation of this idea is of course, the theory of “adrenal fatigue.”
The theory was logical and appeared to make sense on many levels.
Unfortunately, 20 years of research have failed to validate the theory. Moreover, many lines of evidence overtly contradict the notion that adrenal/HPA function or cortisol levels are a primary factor in chronic fatigue/burnout.
The research appears to validate the position held by the Hormone Foundation and Endocrine Society (that represents 14,000 Endocrinologist MDs):
“’Adrenal fatigue’ is not a real medical condition. There are no scientific facts to support the theory that long-term mental, emotional, or physical stress drains the adrenal glands and causes many common symptoms.”
If we are going to truly find effective answers to chronic fatigue, we must let go of outdated concepts that aren’t supported by the evidence. I humbly suggest that if we want to make real progress in helping people with chronic fatigue, we must move beyond the “adrenal fatigue” theory and stop focusing on the adrenals/cortisol as thought it is the central cause in chronic fatigue.
Overall, the body of scientific research suggests that the focus on cortisol levels as the key factor in chronic fatigue is extremely misguided.
My hope is that this review of the research will help to shift the paradigm of how we approach treating chronic fatigue/burnout, and to help individuals struggling with chronic fatigue/burnout to find the best, evidence-based path to fixing their fatigue.
Is Adrenal Fatigue Real? - Sources
[1] Newman T. 2016 Adrenal Fatigue: Does It Exist? What Is Adrenal Insufficiency?
[2] Cadegiani FA et al. (2016) Adrenal fatigue does not exist: a systematic review.
[3] Raikkonen K., et al. (1997) Vital Exhaustion – A Syndrome of Psychological Distress
[4] Adrenal Advice, Symptom Comparison: CFS vs AF
[5] SERTÖZ ÖÖ., et al. The Neurobiology of Burnout: The HypothalamusPituitary-Adrenal Gland Axis and Other Findings
[6] SERTÖZ ÖÖ., et al. The Neurobiology of Burnout: The HypothalamusPituitary-Adrenal Gland Axis and Other Findings
[7] Cleare AJ. (2003) The HPA axis and the genesis of chronic fatigue syndrome
[8] Cleare AJ. (2003) The HPA axis and the genesis of chronic fatigue syndrome
[9] Cleare AJ. (2003) The HPA axis and the genesis of chronic fatigue syndrome
[10] McKenzie, R. MD., et al. (1998) Low-Dose Hydrocortisone for Treatment of Chronic Fatigue Syndrome – A Randomized Controlled Trial
[11] Morris G, et al. (2016) Hypothalamic-Pituitary-Adrenal Hypofunction in Myalgic Encephalomyelitis (ME)/Chronic Fatigue Syndrome (CFS) as a Consequence of Activated Immune-Inflammatory and Oxidative and Nitrosative Pathways.
[12] Morris G, et al. (2016) Hypothalamic-Pituitary-Adrenal Hypofunction in Myalgic Encephalomyelitis (ME)/Chronic Fatigue Syndrome (CFS) as a Consequence of Activated Immune-Inflammatory and Oxidative and Nitrosative Pathways.
[13] Cleare AJ. (2003) The HPA axis and the genesis of chronic fatigue syndrome
[14] Champaneri, S MD et al. (2013) Diurnal Salivary Cortisol is Associated With Body Mass Index and Waist Circumference: The Multi-Ethnic Study of Atherosclerosis
[15] Christianson, A. MD., Why I want to rename adrenal fatigue
[16] Naviaux RK., (2016) Metabolic features of chronic fatigue syndrome
[17] Naviaux RK., (2016) Metabolic features of chronic fatigue syndrome
[18] Cleare AJ. (2003) The Neuroendocrinology of Chronic Fatigue Syndrome
[19] Champaneri, S MD et al. (2013) Diurnal Salivary Cortisol is Associated With Body Mass Index and Waist Circumference: The Multi-Ethnic Study of Atherosclerosis
[20] Abbruzzese EA., et al. (2014) The Influence Of The Chronotype On The Awakening Response Of Cortisol In The Morning
[21] Abbruzzese EA., et al. (2014) The Influence Of The Chronotype On The Awakening Response Of Cortisol In The Morning
[22] BM Kudielka et al. (2005) Morningness and Eveningness: The Free Cortisol Rise After Awakening in “Early Birds” and “Night Owls”
[23] Fries E., et al. (2008) The cortisol awakening response (CAR): Facts and future directions
[24] Oginska H., et al. (2010) Chronotype, sleep loss, and diurnal pattern of salivary cortisol in a simulated daylong driving.
[25] Polugrudov, AS., et al. (2016) Wrist temperature and cortisol awakening response in humans with social jetlag in the North
[26] Kohyama J. (2011) Neurochemical and Neuropharmacological Aspects of Circadian Disruptions: An Introduction to Asynchronization
[27] Oginska H., et al. (2010) Chronotype, sleep loss, and diurnal pattern of salivary cortisol in a simulated daylong driving.
[28] Merikanto I., et al. (2015) Eveningness relates to burnout and seasonal sleep and mood problems among young adults.
[29] Randler C., et al. (2015) Morningness in Teachers is Related to a Higher Sense of Coherence and Lower Burnout
[30] Merikanto I., et al. (2015) Eveningness relates to burnout and seasonal sleep and mood problems among young adults.
[31] Kohyama J. (2011) Neurochemical and Neuropharmacological Aspects of Circadian Disruptions: An Introduction to Asynchronization
[32] Goel N., et al. (2009) Circadian rhythm profiles in women with night eating syndrome.
[33] Sjörs A., et al. Long-term follow-up of cortisol awakening response in patients treated for stress-related exhaustion
[34] Tryon WW., et al. (2004) Chronic fatigue syndrome impairs circadian rhythm of activity level
[35] Fries E., et al. (2008) The cortisol awakening response (CAR): Facts and future directions
[36] Späth-Schwalbe E., et al. (1992) Nocturnal adrenocorticotropin and cortisol secretion depends on sleep duration and decreases in association with spontaneous awakening in the morning.
[37] Leese G., et al. (1996) Short-term night-shift working mimics the pituitary-adrenocortical dysfunction in chronic fatigue syndrome.
[38] Morriss R., et al. (1993) Abnormalities of sleep in patients with the chronic fatigue syndrome.
[39] Fossey M., et al. (2004) Sleep quality and psychological adjustment in chronic fatigue syndrome.
[40] Le Bon O., et al. (2000) How significant are primary sleep disorders and sleepiness in the chronic fatigue syndrome?
[41] Nisenbaum R., et al. (2003) A population-based study of the clinical course of chronic fatigue syndrome
[42] Tell D., et al. (2014) Day-to-day dynamics of associations between sleep, napping, fatigue, and the cortisol diurnal rhythm in women diagnosed as having breast cancer.
[43] Tell D., et al. (2014) Day-to-day dynamics of associations between sleep, napping, fatigue, and the cortisol diurnal rhythm in women diagnosed as having breast cancer.
[44] Fei-Hsiu Hsiao., et al. (2009) The self-perceived symptom distress and health-related conditions associated with morning to evening diurnal cortisol patterns in outpatients with major depressive disorder
[45] Grossi G., et al. (2015) Stress-related exhaustion disorder–clinical manifestation of burnout? A review of assessment methods, sleep impairments, cognitive disturbances, and neuro-biological and physiological changes in clinical burnout.
[46] Leese G., et al. (1996) Short-term night-shift working mimics the pituitary-adrenocortical dysfunction in chronic fatigue syndrome.
[47] McKenzie, R. MD., et al. (1998) Low-Dose Hydrocortisone for Treatment of Chronic Fatigue Syndrome – A Randomized Controlled Trial
[48] Cleare AJ. et al. (1999) Low-dose hydrocortisone in chronic fatigue syndrome: a randomised crossover trial.
[49] McKenzie, R. MD., et al. (1998) Low-Dose Hydrocortisone for Treatment of Chronic Fatigue Syndrome – A Randomized Controlled Trial
[50] Cleare AJ. et al. (1999) Low-dose hydrocortisone in chronic fatigue syndrome: a randomised crossover trial.
[51] Blockmans D., et al. (2003) Combination therapy with hydrocortisone and fludrocortisone does not improve symptoms in chronic fatigue syndrome: a randomized, placebo-controlled, double-blind, crossover study.
[52] Blockmans D., et al. (2003) Combination therapy with hydrocortisone and fludrocortisone does not improve symptoms in chronic fatigue syndrome: a randomized, placebo-controlled, double-blind, crossover study.
[53] Blockmans D., et al. (2003) Combination therapy with hydrocortisone and fludrocortisone does not improve symptoms in chronic fatigue syndrome: a randomized, placebo-controlled, double-blind, crossover study.
[54] McKenzie, R. MD., et al. (1998) Low-Dose Hydrocortisone for Treatment of Chronic Fatigue Syndrome – A Randomized Controlled Trial
[55] McKenzie, R. MD., et al. (1998) Low-Dose Hydrocortisone for Treatment of Chronic Fatigue Syndrome – A Randomized Controlled Trial
[56] Van Den Eede F., et al. (2007) Hypothalamic-Pituitary-Adrenal Axis Function in Chronic Fatigue Syndrome
[57] Morris G, et al. (2016) Hypothalamic-Pituitary-Adrenal Hypofunction in Myalgic Encephalomyelitis (ME)/Chronic Fatigue Syndrome (CFS) as a Consequence of Activated Immune-Inflammatory and Oxidative and Nitrosative Pathways.
[58] Cleare AJ. (2003) The HPA axis and the genesis of chronic fatigue syndrome
[59] Parker AJR., et al. (2001) The neuroendocrinology of chronic fatigue syndrome and fibromyalgia
[60] Tomas C., et al. (2013) A Review of Hypothalamic-Pituitary-Adrenal Axis Function in Chronic Fatigue Syndrome
[61] Grossi G., et al. (2015) Stress-related exhaustion disorder–clinical manifestation of burnout? A review of assessment methods, sleep impairments, cognitive disturbances, and neuro-biological and physiological changes in clinical burnout.
[62] Leese G., et al. (1996) Short-term night-shift working mimics the pituitary-adrenocortical dysfunction in chronic fatigue syndrome.
[63] Christianson A. MD., Kresser C., (2016) Adrenal SummitInterview
[64] Adam EK., et al. (2017) Diurnal cortisol slopes and mental and physical health outcomes: A systematic review and meta-analysis
[65] Adam EK., et al. (2017) Diurnal cortisol slopes and mental and physical health outcomes: A systematic review and meta-analysis
[66] Kudielka BM., et al. (2006) Cortisol in burnout and vital exhaustion: an overview




